Confidential Sexual Health Screening Kit & Tests
You might be reading this after a condom split, before a new relationship, or because something just feels off and you’d rather sort it out privately than sit in a waiting room. That’s common. So is putting testing off because life is busy, clinic times don’t work, or the thought of explaining your sex life to a stranger feels exhausting.
A sexual health screening kit changes that equation. It lets you collect your sample at home, post it to a lab, and get your results securely without arranging a clinic visit first. For many people, that’s the difference between meaning to get tested and doing it.
At-home testing is no longer a niche option. In the Republic of Ireland, free STI home test kit orders rose from 91,000 in 2022 to 126,090 in 2024, a 38.6% increase, showing how quickly people have adopted home screening as part of modern sexual health care (Grand View Research). That matters for UK and Ireland readers because the same practical barriers keep coming up: privacy, time, travel, and wanting fast answers.
If you’ve never used one before, the process can sound more medical than it really is. People often worry about four things:
- Privacy: Will the packaging be obvious?
- Accuracy: Can a home sample really be reliable?
- Timing: When should I test after sex or symptoms?
- What happens next: If I’m positive, do I have to handle treatment alone?
The short answer is no. You don’t have to guess your way through any of that.
Testing from home isn’t about avoiding proper care. It’s often the simplest route into proper care.
A good guide should leave you feeling calmer, not more confused. That means explaining terms like window period in everyday language, showing what’s inside a kit, and making clear how private testing can sit alongside free NHS or HSE treatment pathways.
Taking Control of Your Sexual Health from Home
It is 8:40 pm. The clinic phone lines are closed, you have work in the morning, and you are trying to work out whether testing can wait another week. For many, that is the primary barrier. Not the test itself, but finding a private, practical way to get it done.
Home testing appeals because it fits around ordinary life. You can sort it out after work, avoid the journey to a clinic, and deal with a sensitive health question without explaining it to a receptionist or sitting in a waiting room with neighbours nearby. If you live with family, share a flat, or travel for work, that extra control can make the difference between putting testing off and doing it.
Why home testing feels easier
A home kit reduces the number of steps between concern and action. Order the kit. Collect the sample. Post it back. Read your results securely.
That simplicity matters more than people sometimes realise. Sexual health decisions are often delayed by small practical problems, not lack of common sense. You may need time alone to do a swab, may not want post sent to a shared address without discreet packaging, or may want to avoid missing work for an appointment that could take ten minutes or two hours.
There is also an emotional side to it. Home testing gives you more control over the setting, the timing, and who knows you are testing. For many UK and Ireland readers, privacy is not just about embarrassment. It is about keeping a personal health decision personal.
A private route that can still work with public care
Using a private kit does not cut you off from the NHS or HSE. In many cases, it works alongside them.
A good way to look at it is as a hybrid path. You use a private postal kit to get checked quickly and discreetly, then use NHS or HSE services for follow-up, treatment, or extra support if needed. That can be especially useful if you want to test on your own schedule first, or if local clinic access is limited. If you are comparing options, Repose also explains how private health screening in the UK fits into wider care pathways.
Cost is part of the decision too. Free services remain a strong option, and they matter. Private kits appeal when speed, convenience, choice of panel, or home privacy matter more to you at that moment. The right option is the one you will use.
What taking control really means
Taking control means reducing the gap between wondering and knowing.
That can mean testing after a new partner, after symptoms that do not feel normal, after sex without a condom, or as part of routine screening even when you feel completely well. Some infections do not cause obvious symptoms, which is why waiting for a clear sign can give false reassurance.
It also means knowing that testing is a first step, not a solo project. If a result needs treatment or a clinician review, you still have routes into proper care.
Practical rule: If you keep thinking, “I should probably get tested,” that is usually a good reason to stop delaying it.
Understanding At-Home Sexual Health Screening
The easiest way to think about a sexual health screening kit is this. It’s a private postal route to a laboratory test.
You don’t perform the lab analysis yourself. You only collect the sample at home. The testing still happens in a professional setting after your sample arrives.

What a kit usually includes
Most kits are designed to be simple to use, even if you’ve never done any kind of home test before. Depending on the panel, the box may contain:
- Collection tools such as a urine pot, swab, or finger-prick blood device
- Step-by-step instructions written in plain language
- Labels or ID details so the lab can match your sample correctly
- Return packaging for posting the sample back safely
That’s why many people find the process less intimidating than a clinic appointment. The hard part is often the anticipation, not the sample collection itself.
How it differs from a clinic visit
A clinic visit usually involves travel, timing, registration, and sometimes discussing symptoms face to face before any samples are taken. A home kit strips that back.
The main differences are practical:
- Privacy at home: You choose the setting and timing.
- Less disruption: No need to arrange travel or time off work.
- Straightforward collection: You follow written instructions rather than managing everything in an unfamiliar environment.
If you’re comparing options, Repose Healthcare lists private home testing choices within its wider private health screening in the UK range, which can help you see how sexual health testing fits alongside other at-home diagnostics.
A simple analogy for first-time users
It’s like sending a tracked parcel that happens to contain your sample instead of paperwork.
You’re not replacing clinicians or laboratories. You’re replacing the part that usually slows people down: getting through the clinic door.
That’s also why confusion can crop up. People sometimes assume “at-home test” means “instant result in your bathroom”. Some kits do work that way, but many sexual health screening kits are different. You collect at home, then a lab processes the sample and issues the result.
That distinction matters because it combines convenience with clinical testing standards.
Deciding If At-Home STI Screening Is Right for You
Some people only think about STI testing when they have symptoms. That’s understandable, but it’s not the whole picture.
A lot of infections are quiet at first. No pain. No rash. No obvious warning sign. That means screening is often about being proactive, not reacting to something dramatic.
Situations where testing makes sense
Home screening can be a good fit if any of these sound familiar:
-
Before a new relationship
You both want peace of mind and a more open conversation about sexual health. -
After unprotected sex
You don’t want to sit with uncertainty longer than necessary. -
If something feels different
Maybe there’s discharge, irritation, bleeding, pelvic discomfort, or pain when you pass urine. -
As part of routine care
You’re sexually active and want testing to be a normal health habit, like a dental check or smear reminder. -
If clinics feel hard to access
Work, childcare, travel, or privacy concerns make home testing much more realistic.
Why this matters in the UK
The need for accessible screening is clear. UKHSA reported 440,000 STI diagnoses in 2023, with chlamydia the most common at 217,000 cases. Young people aged 15 to 24 are disproportionately affected (UKHSA).
That doesn’t mean only younger people should test. It means infections are common enough that screening should be viewed as ordinary healthcare, not something reserved for “high-risk” stereotypes.
Common reasons people hesitate
People often delay testing because they tell themselves one of these stories:
-
“I’d know if something was wrong.”
Not always. Some infections don’t cause obvious symptoms. -
“It was only once.”
A single encounter can still be enough to justify a test. -
“I’m embarrassed to order a kit.”
Privacy concerns are real, but they’re also one of the main reasons home testing exists. -
“I’ll book something later.”
Later can easily become weeks or months.
If you’d rather know than wonder, screening is doing its job.
When home testing may not be enough on its own
At-home testing is helpful, but it’s not the answer to every situation.
Seek direct clinical help if you have significant pain, heavy bleeding, ulcers, fever, severe pelvic symptoms, or anything that feels urgent. A kit is useful for screening. It isn’t a substitute for urgent assessment when symptoms are more serious.
For everyone else, a home kit can be the easiest first step because it lowers the barrier between concern and action.
A Look Inside Your Sexual Health Screening Kit
Not every sexual health screening kit looks the same. Some focus on the most common bacterial infections. Others cast a wider net and include blood tests and extra swabs for more complete screening.
That’s why choosing a panel matters. You’re not just buying “a test”. You’re choosing which infections are being checked and what samples you’ll need to provide.
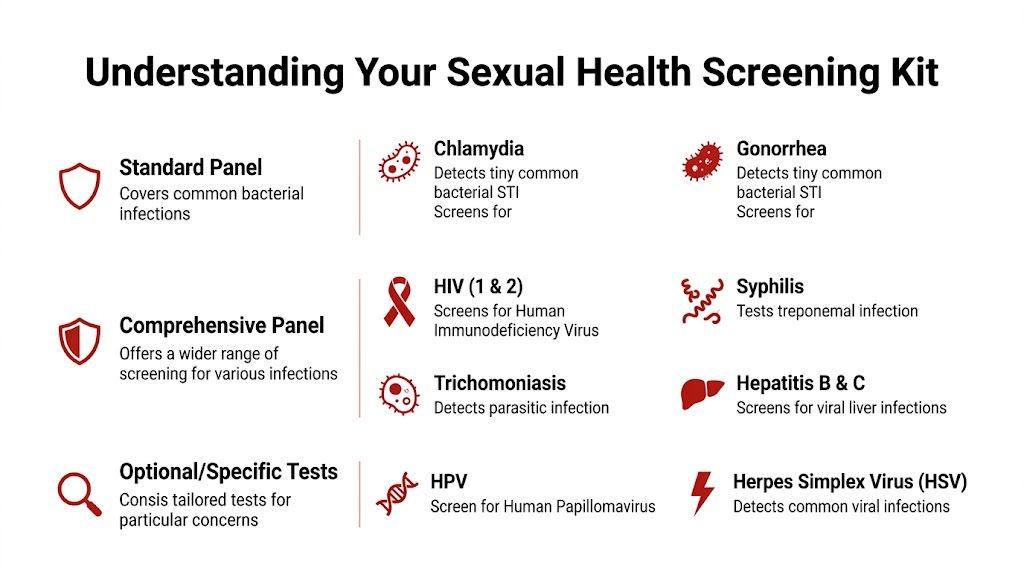
What a panel can include
STI screening kits can process multi-site samples for up to 14-panel detection, including genital, throat, and rectal swabs for infections like Chlamydia and Gonorrhoea, plus blood tests for HIV, Syphilis, and Hepatitis, targeting over 90% of UK STI notifications** (MyLab Box product information).mylabbox.com/product/total-box-14-panel-at-home-std-test-kit/)).
In plain language, that means one kit can involve different sample types for different infections:
- Urine samples are commonly used for some genital infections.
- Swabs may be used for vaginal, throat, or rectal screening.
- Finger-prick blood samples can be used for blood-borne infections.
Basic screen versus full screen
A basic screen usually focuses on common bacterial infections that are often checked first, especially when someone wants a straightforward test after a new partner or a change in symptoms.
A full screen is broader. It’s often a better fit when you want a more complete picture, have symptoms that aren’t specific, or want screening that includes viral and blood-borne infections as well.
One practical way to decide is to ask yourself whether you want the minimum check that answers one immediate concern, or whether you want wider reassurance from one order.
Repose Healthcare STI Test Panels at a Glance
| Infection Screened | Sample Type Required | Included in Basic Screen | Included in Full Screen |
|---|---|---|---|
| Chlamydia | Urine or swab | Yes | Yes |
| Gonorrhoea | Urine or swab | Yes | Yes |
| Trichomoniasis | Swab or urine, depending on kit | No | Often included |
| HIV | Finger-prick blood | No | Often included |
| Syphilis | Finger-prick blood | No | Often included |
| Hepatitis | Finger-prick blood | No | Often included |
| Throat infections such as Chlamydia or Gonorrhoea | Throat swab | Not usually | May be included |
| Rectal infections such as Chlamydia or Gonorrhoea | Rectal swab | Not usually | May be included |
How to choose without overthinking it
A few simple questions help narrow things down:
-
Where was the sexual contact?
Vaginal, oral, and anal sex can affect which sample sites matter. -
Do you have symptoms, or are you screening routinely?
Symptoms may justify a broader panel depending on the situation. -
Do you want a focused answer or wider reassurance?
A basic screen answers common questions. A fuller panel covers more ground. -
Are blood-borne infections part of your concern?
If yes, you’ll want a kit that includes finger-prick blood collection.
Why the contents can feel unfamiliar
People are often surprised that one kit may include more than one type of collection tool. That’s normal.
Different infections are best detected from different sample types, which is why a kit testing for more infections can look a bit more involved at first glance. In practice, the instructions usually break each part down into simple actions, one at a time.
Your Simple Journey from Order to Results
Knowing the order of events can bring a sense of calm. The process is usually much simpler than they expect.

Step 1 Order your kit
You choose the test online based on the kind of screening you want. If you already know you want a home option, you can order an STI test online and have the kit delivered to your address.
For many users, this is the point where anxiety drops. Once the order is placed, you’ve moved from worrying to doing something useful.
Step 2 Collect your sample
When the kit arrives, read the instructions before opening every packet.
That sounds obvious, but it helps. Most collection mistakes happen when people rush.
A few practical examples:
- Urine sample: You may be asked to collect the sample in a specific way and transfer it carefully.
- Swab sample: You’ll follow the printed steps for the relevant body site.
- Finger-prick blood: Warm hands and taking your time often make the process easier.
Step 3 Return it to the lab
After collection, you package the sample as instructed and post it back using the return materials provided.
This step matters because a well-labelled and promptly returned sample gives the lab the clearest possible starting point. If you’re in a more remote area, it’s sensible to post as soon as you can rather than leaving the kit sitting around.
Step 4 Check your results securely
Once the laboratory has processed the sample, results are shared through a secure online system.
At this stage, desired outcomes generally fall into one of three categories:
- Clear confirmation that everything is negative
- A straightforward explanation of any positive result
- Guidance on what to do next
Don’t leave a completed sample on the side because you’re nervous about the answer. The delay won’t change the result. It only delays your next step.
Small choices that make the process smoother
- Pick a calm time: Don’t collect samples while rushing out the door.
- Read every label: Make sure names or reference details are correct where needed.
- Post promptly: Faster return reduces unnecessary delay.
- Check your email or dashboard access: Make sure you can receive the result notification.
A sexual health screening kit works best when you treat it like any other health task. Follow the steps carefully. Keep it simple. Get it done.
Understanding Your Test Results and Next Steps
You log in, your stomach drops, and then you see a result you were not fully prepared for. That reaction is common, whether the answer is negative, positive, or unclear.
Knowing what the wording means can make that moment easier to handle.

What accuracy really means
No test is perfect, but good laboratory testing is designed to answer two practical questions clearly.
- Sensitivity means how well a test picks up an infection when it is present.
- Specificity means how well a test avoids marking someone as positive when they do not have that infection.
If those terms feel technical, focus on their practical meaning. A highly sensitive test misses fewer true infections. A highly specific test produces fewer false positives. That is why results should always be read alongside timing, symptoms, and any recent exposure.
What a window period means
A window period is the time between catching an infection and the point when a test can detect it reliably.
This is one of the easiest places to get tripped up. You can test too soon, receive a negative result, and still need another test later. Window periods work a bit like taking a photo before the image has come into focus. The exposure may have happened, but the test may not yet have a clear enough signal to detect it.
If you are unsure about timing, sample type, or when results are usually released, Repose Healthcare explains the process in this guide to how long STI test results take.
How to act on different result types
Negative result
A negative result is reassuring, but it only answers the question for the infections included in that kit and the point in time when you tested.
Three checks help here. Did you test after the right window period? Did you use the right sample site, such as urine, vaginal swab, throat swab, or rectal swab if relevant? Have you had any new sexual contact since taking the sample?
If any of those answers are uncertain, repeat testing may be sensible. Private and public systems can work well together in these circumstances. You might use a private kit for speed and privacy at home, then use NHS or HSE services for follow-up if symptoms continue, if you need an examination, or if you want a clinician to review ongoing risk.
Positive result
A positive result gives you a clear next job. Get treatment or confirmatory follow-up, depending on the infection and the advice provided.
Try to keep your response practical.
- Pause sexual contact until you have clear guidance on treatment and when it is safe to resume
- Arrange treatment quickly, either through a private provider or through NHS or HSE sexual health services
- Tell recent partners if the advice says they may need testing or treatment
- Read the notes carefully, because some infections need repeat testing or extra checks
A private kit can be the first step, not the whole journey. For many people in the UK and Ireland, the easiest route is hybrid. Test privately if cost, speed, or home privacy suits you better, then use free NHS or HSE treatment pathways where appropriate. That can save time without losing access to public care.
STIs are health issues. They are treatable, manageable, and common reasons to seek care.
Inconclusive or invalid result
An inconclusive or invalid result usually points to a sample issue rather than a diagnosis. The sample may not have been suitable for processing, or the lab may not have had enough material to give a reliable answer.
The usual next step is simple. Retest, and follow the collection instructions closely.
If privacy worries are part of why you chose home testing in the first place, that concern can continue after the result too. People sometimes also want advice on removing personal data from wider online sources, especially if they are thinking carefully about digital privacy as well as medical confidentiality.
How Repose Healthcare Protects Your Data and Privacy
Privacy is often the deciding factor for people considering a sexual health screening kit. They’re not only thinking about the result. They’re thinking about the parcel on the doormat, the lab process, the digital record, and who else might see any of it.
That concern is reasonable.
What confidentiality looks like in practice
A private testing service should make confidentiality part of the process from the start, not an afterthought.
That usually means thinking about privacy at several points:
- Delivery privacy so the outer packaging doesn’t reveal sensitive medical details
- Sample privacy so the lab can process the sample using the correct identifiers
- Results privacy so access is restricted to the right person
- Data handling privacy so information is managed under GDPR rules
For many users, the parcel itself causes the first worry. If you live with parents, children, a partner, or flatmates, you don’t want the packaging to announce what’s inside.
Why digital privacy matters too
People often focus on the test but forget the account behind it.
Good digital hygiene matters on your side as well:
- Use a private email account you can access easily
- Choose a secure password for any health dashboard
- Log out on shared devices
- Keep result notifications private if others can see your lock screen
If you’re generally concerned about your digital footprint beyond healthcare, guides on removing personal data can help you understand the wider steps people take to reduce what’s publicly visible online.
The key reassurance
A confidential sexual health service should minimise unnecessary exposure at every stage.
That means you shouldn’t have to choose between getting tested and protecting your privacy. A well-designed home testing process should support both.
Your Questions on Sexual Health Screening Answered
Some of the most important questions only come up once you’re close to ordering.
Can I use a private kit and still get free treatment?
Yes. That’s one of the most useful things to understand.
Amid NHS clinic waits of 14 to 21 days, private kits can offer a faster route to screening, and a positive result from a private kit qualifies a user for free NHS treatment and partner notification services (PMC article).
That creates a practical hybrid path. You pay for speed and privacy at the testing stage, then use the public system for treatment and follow-up where appropriate.
Will my GP be told automatically?
Not usually as an automatic assumption for every private test result, but follow-up care may involve sharing information if treatment or onward clinical support is needed.
If that matters to you, check the provider’s privacy and reporting policy before ordering.
What if I collect the sample incorrectly?
That can happen, especially with first-time users.
Most issues are fixable. If a sample is invalid or inconclusive, you’ll usually be told that the result isn’t clear rather than being given a misleading answer. Read the instructions slowly, wash your hands, label things carefully, and don’t rush.
Can I use a sexual health screening kit anywhere in the UK or Ireland?
Services vary by provider, but many at-home kits are designed for people across the UK and Republic of Ireland.
If you live in a remote area, post the sample promptly and follow any instructions about storage and return timing.
Is a home kit enough if I have symptoms?
Sometimes yes, sometimes no.
If symptoms are mild and you mainly need screening, a kit can be a useful first step. If symptoms are severe, rapidly worsening, or you feel unwell, seek direct medical care instead of waiting on postal testing.
Is paying for a private test worth it if NHS or HSE options exist?
That depends on what you need most right now.
If your priority is no-cost testing, free services may suit you. If your priority is privacy, convenience, or getting started quickly while public services are busy, a private kit can be a practical option. For many people, it isn’t an either-or decision. It’s a staged approach.
If you want a discreet, practical way to get started, Repose Healthcare offers at-home health testing for people across the UK and Republic of Ireland, including sexual health screening options with secure results and clear next-step information.


You Might Also Like
The 2026 Cost of Hepatitis Vaccination in the UK
You're usually looking up the cost of hepatitis vaccination for a practical reason. A trip [...]
Hormone Blood Test London: Find Your Perfect Test
Some London health questions start subtly. Your cycle changes a little. You feel wired at [...]
Peanut Allergy Test Kit: A Practical UK User’s Guide
A peanut reaction often starts with uncertainty, not clarity. You eat a biscuit, satay sauce, [...]
NIPT Test Edinburgh: Your 2026 Guide
If you're searching nipt test edinburgh, you're probably already in that familiar stage of pregnancy [...]
Peripheral Artery Disease UK: Peripheral Artery Disease UK:
You might be reading this because walking has started to feel different. Perhaps your calf [...]
NIPT Test Cardiff: Clinic, Home & NHS Pathways 2026
If you're in Cardiff, newly pregnant, and staring at screening options that all seem to [...]
Gender Scan Difference UK: Accuracy, Timing & Cost Compared
You've probably already done the same search most parents do. One tab shows the NHS [...]
NIPT Test Cambridge: Guide to Options & Booking 2026
You're in Cambridge, you've had the first rush of finding out you're pregnant, and then [...]
Home COVID Test Results: A Practical UK & Ireland Guide
You've done the swab, mixed the sample, added the drops, and now you're staring at [...]
DVT Test Squeeze Calf: Homan’s Sign & Beyond
You notice one calf is sore, a little swollen, and not behaving like an ordinary [...]
Your Guide to Every Travel Clinic Leicester Offers in 2026
Flights are booked. The hotel is sorted. Your passport is still in date. Then one [...]
13 Week Gender Scan: Accuracy, NIPT & What to Expect
By the time you reach 13 weeks, pregnancy often starts to feel more real in [...]
Your Pregnancy Scan London: Guide to Options & Costs
A positive test can make London feel suddenly very small and very complicated. You might [...]
Your Nuchal Dating Scan Explained: A 2026 UK Guide
That appointment message has landed in your phone or come through the post, and suddenly [...]
Normal Cortisol Levels UK: Get Clarity
Some people search for normal cortisol levels uk after weeks of feeling unlike themselves. They’re [...]
How to Test Iron Levels in Blood: A Complete UK Guide
You’re probably not searching how to test iron levels in blood out of curiosity. More [...]
Growth Scan Pregnancy: UK Guide & What to Expect
You’re at an antenatal appointment, everything seems routine, and then your midwife says, “We’d like [...]
Gender Scan Near Me: Your 2026 Guide to Options
You’re probably here because the question has stopped feeling abstract. Maybe you’ve had your booking [...]
Progesterone Test For Pregnancy: Viability & Home Kit
The positive test is there, but relief doesn’t always follow. For many women, early pregnancy [...]
Ovulation Blood Tests: Confirm Your Ovulation
You’ve probably already done some version of this. You’ve checked an app, watched for a [...]
How to Test Testosterone Levels: A UK Guide
You wake up tired, despite a full night in bed. Your training feels flat. Your [...]
UK Vitamin D Test: A Complete At-Home Guide for 2026
You wake up tired, even after a full night’s sleep. By mid-afternoon you’re reaching for [...]
Blood Iron Level Test: A Complete UK Guide for 2026
Some days it isn’t dramatic. You’re just slower than usual. You wake up after a [...]
Cortisol Levels Test: Your Comprehensive UK Guide
You wake up tired, push through the morning on caffeine, feel oddly tense by midday, [...]
Travel Clinic Leeds: Compare 7 Top Options For 2026
You book the flights first. Then the practical questions start. Is a tetanus booster enough [...]
Private Blood Test Leicester: A Complete 2026 Guide
You wake up tired again. Maybe you’ve had weeks of bloating, odd fatigue, headaches, low [...]
Genetic Testing Before Pregnancy: A UK Guide for 2026
You might be at the stage where baby plans still live in half-finished conversations. One [...]
Harmony NIPT Test: A Clear Guide for Expectant Parents
You may be sitting with a booking slip from your midwife, a browser full of [...]
Decode Your Health: Understanding Full Blood Count Results
That moment is familiar. You open your blood test report on your phone, see a [...]
Iron Level Tester: Your Guide to Better Health
You wake up tired, push through the day with coffee, and still feel flat by [...]