Genetic Testing Before Pregnancy: A UK Guide for 2026
You might be at the stage where baby plans still live in half-finished conversations. One of you mentions names. The other starts thinking about finances, work, and whether now is the right time. Then a new question appears: is there anything sensible we can do before pregnancy to understand genetic risks?
That’s where genetic testing before pregnancy can help. It doesn’t predict everything about a future child, and it isn’t a guarantee of a problem or a guarantee of safety. What it does offer is earlier information, while you still have time to think clearly and make choices without the pressure of an ongoing pregnancy.
For many couples in the UK and Ireland, access is part of the problem. NHS services can be excellent, but they’re often focused on people who meet strict referral criteria or have a known family risk. Demand also exceeds capacity. Average waits for genetic counselling often exceed 6 to 12 months, and only 15% of eligible couples access expanded carrier screening before conception via the NHS, according to a 2024 report discussed in this UK access analysis. If you’re trying to plan around age, fertility treatment, work leave, or your own readiness, that delay can feel enormous.
It’s one reason many people now build preconception health planning in layers. They look at supplements, cycle tracking, medical history, and practical resources such as this ultimate pregnancy preparation checklist, then add genetic screening if they want a clearer picture before trying to conceive.
Planning Your Family’s Future An Introduction
Sophie and Mark have been talking about trying for a baby later this year. Neither has a known genetic condition in the family. They’re healthy, busy, and a bit overwhelmed by the amount of conflicting advice online. They assumed genetic testing was only for people with a strong family history, or something offered once pregnancy had already started.
That assumption is very common.
Pre-pregnancy genetic testing is often less dramatic than people expect. In most cases, it’s carrier screening. That means checking whether you carry a gene change for an inherited condition that could be passed on if your partner carries a change in the same gene too. Most carriers are completely healthy and would never know without testing.
The emotional side matters here. Couples often feel two things at once. They want reassurance, and they’re worried that testing will create more anxiety. Both reactions make sense. Good preconception care isn’t about collecting frightening information. It’s about replacing uncertainty with something more useful: context, options, and time.
In the UK especially, timing changes the conversation. NHS pathways are usually aimed at people with a clear reason for referral, such as family history or membership of a higher-prevalence group for certain conditions. Many others don’t meet the threshold, or they do qualify but face long waits.
Early information is often calmer information. You have more time to ask questions, involve your partner, and decide what matters to your family.
That’s why at-home testing has become part of real-world family planning. For couples who want privacy, convenience, and control over timing, it can bridge a gap that public services don’t always fill quickly enough.
What Is Pre-Pregnancy Genetic Testing
Pre-pregnancy genetic testing usually refers to carrier screening. The goal is simple. It checks whether you or your partner carry inherited gene changes that could matter if you have a child together.
For many couples, that sounds more alarming than it is.
A carrier is usually a healthy person who happens to have one altered copy of a gene linked to a recessive condition. Because the other copy still does its job, there are often no symptoms and no reason you would ever suspect anything from your own health or family history.

What being a carrier means
The key point is that carrier results are interpreted as a pair, not in isolation. If both partners carry a change in the same recessive gene, there is a chance of having an affected child. If only one partner is a carrier for that condition, the usual concern is much lower.
A helpful way to view it is as a compatibility check between two sets of genetic information. The test is not asking, “Are you healthy?” It is asking, “Could the same condition be passed down from both sides of the family?”
That distinction matters because a carrier result is not a diagnosis. It does not say that you have a disease, and it does not say a future child will definitely have one. It flags a specific reproductive risk so you have time to ask questions, test a partner if needed, and consider your options before pregnancy rather than in the middle of it.
How this differs from testing during pregnancy
Pre-pregnancy testing looks at the adults planning a pregnancy. It focuses on inherited risks that may be present before conception even happens.
Testing during pregnancy answers a different set of questions. It may look for signs that a fetus could have a condition, or it may be used after a scan or screening result suggests something needs a closer look. By that stage, decisions often feel more urgent.
That timing is one reason many people in the UK and Ireland look into testing before trying to conceive. NHS access can be limited by referral rules, ancestry criteria, family history, or waiting lists. At-home screening has become a practical option for couples who want earlier answers without waiting for a clinic pathway to open up.
If you want a plain-English overview of sample analysis, sequencing, and reporting, this guide on how genetic testing works explains the process clearly.
Practical rule: Pre-pregnancy carrier screening helps you plan ahead. It cannot predict every outcome, but it can make the next decision clearer.
Why broader screening matters
Older tests often checked for a small number of conditions linked to a known family history or a specific ethnic background. Expanded carrier screening looks across a wider range of recessive and X-linked conditions, including some that may never have appeared openly in either family.
That is part of why preconception testing has become more relevant outside specialist genetics clinics. Many carriers are identified in families with no known warning signs at all.
For couples deciding whether to try naturally, seek partner testing, speak to a genetic counsellor, or explore fertility options, the value of testing is rarely just the laboratory result. It is the chance to make those choices with more time, more privacy, and less pressure.
Key Types of Genetic Tests for Family Planning
A couple might arrive at this stage thinking they need "the genetic test" before pregnancy, then find three or four very different options with similar-sounding names. That confusion is common. Each test answers a different question, and the right choice depends on what you are trying to plan for.
This visual summary helps separate the main categories.
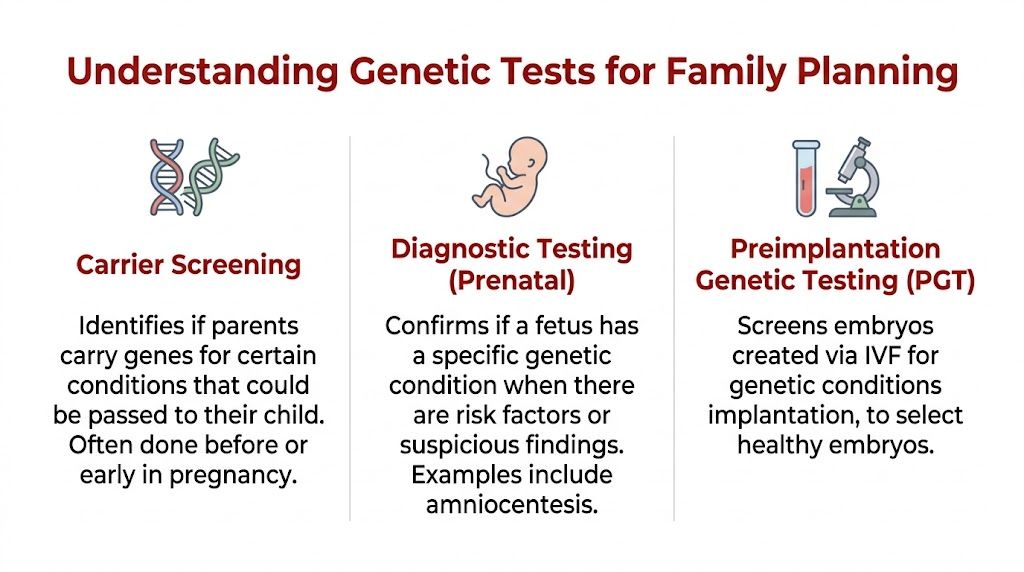
Carrier screening and expanded carrier screening
For people planning a pregnancy, carrier screening is usually the main test to understand first.
Carrier screening asks whether either partner carries gene changes linked to inherited conditions that could be passed on to a child. A smaller, targeted panel checks a limited set of conditions, often based on ancestry or known family history. Expanded carrier screening looks at a wider list of recessive and X-linked conditions, including some that may never have appeared clearly in either family.
That wider reach matters because family history is often an incomplete guide. Some conditions stay hidden for generations because carriers are healthy and never know they carry a gene change. Research discussed in npj Genomic Medicine coverage via ScienceDaily showed that broader testing can detect reproductive risk in both related and unrelated couples, while also showing a significant limitation of smaller panels that only assess more common genes.
A negative result can be reassuring, but it has a specific meaning. It means no relevant carrier finding was identified in the genes and conditions that particular panel examined. It does not mean zero genetic risk.
That distinction is easy to miss.
It also helps explain why some couples in the UK and Ireland choose broader at-home screening. If NHS access is delayed, or if you do not meet local referral criteria, the practical question becomes less about whether testing exists and more about which panel gives you useful information before you start trying.
Medical-grade screening and consumer DNA kits
Consumer DNA kits and clinical carrier screening are not interchangeable.
An ancestry or trait test may offer interesting personal information, but it is not usually built for reproductive decision-making. Clinical screening uses validated laboratory methods, defined condition lists, and reporting standards designed for health use. If you are making choices about trying naturally, testing a partner, or speaking with a genetics professional, that difference matters.
Couples sometimes come across other tests at the same time and assume they are part of the same category. They are not. For example, sperm DNA quality and inherited carrier status are separate questions. This overview of the DNA sperm fragmentation test can help if you are trying to place male fertility testing alongside genetic screening without mixing the two up.
Other tests couples may hear about
Some tests look for single-gene inherited conditions. Others look at chromosomes, a developing pregnancy, or embryos created through IVF. Here is a simple comparison:
| Test type | What it looks for | When it’s usually relevant |
|---|---|---|
| Carrier screening | Whether a parent carries gene changes linked to inherited conditions | Before pregnancy or early in pregnancy |
| Karyotyping | Large-scale chromosome differences in number or structure | Recurrent miscarriage, infertility, or known chromosome concerns |
| Prenatal diagnostic testing | Whether a fetus has a specific genetic condition | During pregnancy when there are risk factors or concerning findings |
| PGT-M | Genetic testing of embryos created through IVF | When a known inherited risk has already been identified |
Karyotyping is a good example of why names alone can be misleading. It examines chromosomes at a broad level rather than checking many individual genes. That makes it useful in some fertility or miscarriage investigations, but it does not replace carrier screening.
A good test answers the question you have. Before you choose one, it helps to ask: are we checking inherited carrier status, chromosome differences, pregnancy findings, or embryo genetics? Once that is clear, the options become much easier to compare.
Who Should Consider Genetic Testing Before Pregnancy
You may be sitting at the kitchen table talking about names, timing, and whether now is the right moment to try for a baby. Then a practical question comes up. Should we do any genetic testing first, even if nothing in our family history seems unusual?
For many couples, that is the right question.
Carrier screening is often associated with families who already know about an inherited condition. Those families are certainly part of the picture. But pre-pregnancy testing is not only for people with an obvious warning sign. It can also help couples who want clearer information before conception, especially in the UK and Ireland, where NHS access may depend on referral criteria and waiting times.
People who have a clear reason to consider testing
Testing is more strongly considered when there is a known clue that inherited risk may be higher. For example:
- A family history of a genetic condition. This includes a close relative with a diagnosed inherited disorder, or a wider family pattern that has already raised concern.
- A previous pregnancy affected by a genetic condition. If this has happened before, testing before another pregnancy can help you understand recurrence risk and your options.
- A community or ancestry group with higher rates of certain conditions. Some inherited conditions are more common in particular populations, so screening may be offered or discussed more readily.
- A relationship between blood relatives. If partners are biologically related, they are more likely to carry the same recessive gene change, which increases the chance of a child inheriting that condition from both sides.
These are the situations most likely to be recognised quickly in traditional medical pathways.
Why people without a family history still ask about testing
Here is the part that often surprises couples. A normal family history does not rule out carrier status.
Recessive conditions can pass undetected through generations because carriers are usually healthy. In other words, a family can carry a gene change for years without anyone knowing it is there. The first sign may only appear when two carriers have a child together.
A simple way to picture this is a set of instructions copied through a family line. If just one copy contains a change, the person carrying it is often completely well. If both parents happen to carry a change in the same gene, that shared risk becomes relevant for pregnancy planning.
That is why some couples choose screening even when no doctor has flagged them as high risk. They are not looking for bad news. They want time to think clearly, ask questions, and make decisions before pregnancy adds urgency.
Who may especially value early, private access
In the UK and Ireland, access is part of the decision.
Some couples meet NHS criteria quickly. Others do not, even though they would still find the information useful. Some are told to wait. Some are advised testing is only indicated after a family history review, fertility concern, or affected pregnancy. If your timeline matters, that gap can feel frustrating.
At-home preconception screening can help in that situation. It gives couples a way to check carrier status earlier, from home, without waiting for multiple appointments just to find out whether testing is available.
You might want to consider it if:
- you want information before trying to conceive, rather than after pregnancy has begun
- you expect NHS waiting times to delay your plans
- you do not meet strict referral criteria but still want to understand shared carrier risk
- you would prefer time to consider partner testing, specialist advice, or reproductive options in a calm way
You do not need a dramatic family history to ask sensible questions about future children.
For some couples, results confirm there is nothing further to do. For others, one partner is found to be a carrier and the next step is testing the other partner. For a smaller group, both partners carry changes in the same gene, which opens a more detailed conversation about reproductive choices.
Each of those outcomes can be useful. The value of testing is not only in finding a problem. It is in getting information early enough to use it.
The At-Home Testing Process From Order to Results
You order a kit on a Tuesday evening after work. By the weekend, the sample is back in the post. A short time later, you have an answer that can shape what happens next, without first waiting months to find out whether you qualify for testing through the NHS or HSE pathway.
That speed is a big part of the appeal in the UK and Ireland. For couples who want information before pregnancy, at-home testing can turn a vague plan into a clear process.

What usually happens step by step
The process is usually simpler than people expect. It works a bit like any other home health kit, but with tighter identity checks because the laboratory needs to match the sample to the right person.
-
You order the kit online.
This is usually the first practical difference from a clinic-based route. You can start from home, on your own timeline, rather than waiting for an appointment just to discuss whether testing is available. -
You register the kit and confirm your details.
This links the sample to you and helps the laboratory process it safely. Take your time here. Small errors, such as entering the wrong date of birth or sample code, can delay the result. -
You collect your sample at home.
Many carrier screening kits use saliva. The instructions often ask you not to eat, drink, smoke, or chew gum for a set period beforehand. That is not a trick step. It helps the lab get enough clean DNA to analyse. -
You send the sample back.
Return packaging is often included, which keeps things straightforward. Post it as soon as you can so the sample reaches the lab in good condition. -
The laboratory analyses the DNA.
The lab looks for specific genetic changes linked to the conditions included on the panel. As noted earlier, recent reporting on direct-to-consumer carrier screening has described growing private uptake alongside concerns about anxiety when counselling is missing. That is why the quality of follow-up matters as much as the lab process itself. -
You receive your results securely.
Results are usually shared through a secure online portal or by a clinician-linked service. Some providers also explain whether partner testing, a repeat sample, or genetic counselling is recommended.
What can slow things down
At-home testing is convenient, but it is not instant.
Delays usually happen for practical reasons. The sample may not contain enough DNA. The registration details may not match. The lab may ask for a repeat sample if the saliva tube was not filled correctly. None of this means something is wrong with your genetics. It usually means the laboratory needs a clearer sample before it can report accurately.
This is one of the biggest misunderstandings couples have. A delayed result is usually an admin or sample-quality issue, not a hidden sign of bad news.
Common concerns before you order
A few questions come up again and again.
-
Will I do the sample correctly?
In most cases, yes. Kits are designed for home use, and the instructions are usually very clear. -
Is saliva really enough?
For many carrier screening panels, yes. The test is built for that sample type. -
Who gets access to the result?
Reputable providers use secure systems and explain their privacy process before you buy. -
What if the result is unclear?
You may be asked to repeat the sample, or you may be offered a follow-up conversation to explain what the laboratory found and what to do next.
A helpful way to judge an at-home test is to look beyond the order page. Check what conditions are included, whether the lab is properly accredited, how results are delivered, and whether real clinical support is available if one of you is found to be a carrier. That support matters especially in the UK and Ireland, where at-home testing often fills the gap before public-system access catches up.
How to Interpret Your Genetic Test Results
This is often the moment people dread. The report arrives. There are gene names, technical terms, and unfamiliar wording. It’s easy to assume the worst if you don’t know what the categories mean.
Most carrier screening reports can be understood by sorting them into a few practical outcomes.
If no carrier status is detected
This usually means the test did not identify a relevant carrier result for the conditions on that panel.
That can be reassuring, but it’s not the same as saying there is zero genetic risk. No test can rule out every inherited condition. Some genes remain undiscovered, and some conditions fall outside the scope of a panel.
A “clear” result reduces known risk for the screened conditions. It does not promise a risk-free pregnancy.
That distinction matters because people sometimes read “not detected” as “impossible”. It’s better understood as “nothing significant was found within the test’s limits”.
If one partner is found to be a carrier
This is common, and on its own it usually says nothing bad about your own health.
The next question is whether your partner carries a change in the same gene. If not, the chance of having a child affected by that specific recessive condition is usually much lower. If partner testing hasn’t happened yet, that’s often the next practical step.
Many people need reassurance here. A carrier result can sound alarming, but being a carrier is not a diagnosis and usually doesn’t mean you will develop the condition yourself.
If both partners are carriers for the same condition
This is the result that changes planning most clearly. It doesn’t tell you what you must do. It tells you that you have a specific inherited risk that deserves a careful conversation.
At that point, couples usually want answers to these questions:
- What exactly is the condition?
- How severe is it, and how variable can it be?
- What reproductive options are available?
- Do we want to conceive naturally, use IVF with embryo testing, consider donor eggs or sperm, or plan for prenatal testing later?
Specialist support helps. If you’re trying to understand how accuracy and screening limits are discussed more broadly in pregnancy-related genetics, this explainer on NIPT test accuracy is useful for learning how screening and diagnostic certainty differ.
A simple way to read the report
| Report wording | What it usually means in plain English |
|---|---|
| No carrier status detected | No relevant finding was identified for the genes and conditions screened |
| Carrier detected | You carry a gene change linked to a condition, usually without it affecting your own health |
| Partner testing recommended | The result only becomes more informative once both partners’ results are considered |
| Shared carrier risk identified | Both partners carry changes in the same condition area and should discuss reproductive options |
Take your time with results. You don’t need to make instant decisions on the day you open the report.
Navigating Next Steps Costs and Access in the UK
A couple in their early thirties gets a carrier result on a Tuesday evening. By Wednesday morning, the science is no longer the confusing part. The practical questions take over. Can we get partner testing quickly? Will the NHS offer follow-up? How much will private testing cost if we do not meet referral criteria?

In the UK and Ireland, access often shapes decisions as much as the result itself. Some couples can use NHS or public hospital pathways. Others find that waiting times, local referral rules, or narrow eligibility criteria make at-home private testing the faster first step. That does not replace specialist care. It often helps you reach the right conversation sooner.
If your result shows no shared concern
If screening does not find a relevant carrier issue, many couples feel able to plan with less uncertainty. Keep that report somewhere easy to find. A digital copy saved with your health records can be helpful later if you speak with a GP, fertility clinic, or maternity team.
A clear result is useful, but it is not a promise about every genetic condition. It is closer to crossing several major items off a checklist than proving the checklist is empty.
If one partner is found to be a carrier
The next step is usually straightforward. Test the other partner if they have not already been screened.
Access has tangible implications. If you are hoping to conceive soon, a delay of weeks or months can matter emotionally and practically. Public services may be available, but they are not always quick, and some couples are told they do not qualify without a stronger family history or another clinical reason. At-home testing can bridge that gap by letting you start partner screening without waiting for a referral.
If both partners carry variants linked to the same condition
At that point, specialist advice matters because the question changes from "What did the test find?" to "What are our options now?" Couples may consider natural conception with a clear understanding of risk, prenatal testing during pregnancy, donor sperm or donor eggs, or IVF with PGT-M.
PGT-M works like a sorting step during IVF. Embryos are created first, then tested for the specific inherited condition before transfer. It is not the right path for every couple, and it brings extra cost, appointments, and decisions, but some families value having that option on the table.
Private screening can also lead into NHS care later. A result from an at-home service may help you have a more focused discussion with your GP or fertility specialist about referral routes, confirmatory testing, counselling, or reproductive treatment.
A shared carrier result does not close doors. It gives you a clearer map.
Cost, waiting times, and what to compare
Price matters, but the cheapest option is not always the most useful one. Two tests can look similar on the surface and differ in ways that affect what happens after the result arrives.
If you want a practical starting point, compare current genetic testing costs in the UK alongside likely turnaround times, whether both partners are included, and what support is offered after a positive result.
Check these points carefully:
- Which conditions are included: A small targeted panel and a broad carrier screen answer different questions.
- How the sample is collected: Saliva kits are common for at-home testing, but some providers use blood samples.
- Which laboratory processes the test: Look for clear information about accreditation and quality standards.
- What happens after a result: Some services include genetic counselling or partner follow-up, while others only issue a report.
- How results are stored and shared: Privacy, secure portals, and GP-friendly reports all make a difference.
For many couples in the UK and Ireland, the comparison is not private versus NHS in abstract terms. It is speed versus waiting, broad access versus strict criteria, and immediate clarity versus uncertainty that drags on while you are trying to make family planning decisions.
Practical Questions About Preconception Screening
Below are some of the questions couples ask most often when they’re deciding whether to go ahead.
| Question | Answer |
|---|---|
| Do both partners need testing at the same time? | Not always. Some couples start with one partner and then test the other if a carrier result appears. Others prefer both partners tested from the outset to avoid delays. |
| Can I do this if I’m not trying yet? | Yes. Many people choose screening well before trying to conceive because it gives them more space to think about the result. |
| Will a carrier result affect my own health? | Usually, no. Carrier screening is mainly about reproductive risk, not about predicting that you will become unwell. |
| What if I have no family history? | You can still be a carrier. Family history can be helpful, but its absence doesn’t rule out inherited risk. |
| Is at-home testing private? | Reputable providers use secure registration and protected online reporting. It’s still worth checking privacy terms before ordering. |
| Should I be worried about feeling anxious while waiting? | It’s normal to feel unsettled. The best safeguard is choosing a service that explains what the result means and where to go next if anything is found. |
| Can people in Ireland use UK-based at-home testing services? | Some UK providers also serve the Republic of Ireland, but shipping, return logistics, and availability can differ, so check before ordering. |
| What if my result shows a shared carrier risk? | Pause, read the report carefully, and seek counselling or specialist advice. That result is important, but it still leaves you with several possible family planning routes. |
Preconception screening works best when you see it for what it is: an information tool. It can reassure, it can redirect, and sometimes it can uncover a risk that deserves a more careful plan. None of those outcomes means you’ve failed. It means you’ve chosen to prepare.
If you want a convenient way to explore genetic testing before pregnancy from home, Repose Healthcare offers UK-based at-home testing with clear instructions, secure results delivery, and clinically focused diagnostics designed to help you make informed next-step decisions with more confidence.


You Might Also Like
The 2026 Cost of Hepatitis Vaccination in the UK
You're usually looking up the cost of hepatitis vaccination for a practical reason. A trip [...]
Hormone Blood Test London: Find Your Perfect Test
Some London health questions start subtly. Your cycle changes a little. You feel wired at [...]
Peanut Allergy Test Kit: A Practical UK User’s Guide
A peanut reaction often starts with uncertainty, not clarity. You eat a biscuit, satay sauce, [...]
NIPT Test Edinburgh: Your 2026 Guide
If you're searching nipt test edinburgh, you're probably already in that familiar stage of pregnancy [...]
Peripheral Artery Disease UK: Peripheral Artery Disease UK:
You might be reading this because walking has started to feel different. Perhaps your calf [...]
NIPT Test Cardiff: Clinic, Home & NHS Pathways 2026
If you're in Cardiff, newly pregnant, and staring at screening options that all seem to [...]
Gender Scan Difference UK: Accuracy, Timing & Cost Compared
You've probably already done the same search most parents do. One tab shows the NHS [...]
NIPT Test Cambridge: Guide to Options & Booking 2026
You're in Cambridge, you've had the first rush of finding out you're pregnant, and then [...]
Home COVID Test Results: A Practical UK & Ireland Guide
You've done the swab, mixed the sample, added the drops, and now you're staring at [...]
DVT Test Squeeze Calf: Homan’s Sign & Beyond
You notice one calf is sore, a little swollen, and not behaving like an ordinary [...]
Your Guide to Every Travel Clinic Leicester Offers in 2026
Flights are booked. The hotel is sorted. Your passport is still in date. Then one [...]
13 Week Gender Scan: Accuracy, NIPT & What to Expect
By the time you reach 13 weeks, pregnancy often starts to feel more real in [...]
Your Pregnancy Scan London: Guide to Options & Costs
A positive test can make London feel suddenly very small and very complicated. You might [...]
Your Nuchal Dating Scan Explained: A 2026 UK Guide
That appointment message has landed in your phone or come through the post, and suddenly [...]
Normal Cortisol Levels UK: Get Clarity
Some people search for normal cortisol levels uk after weeks of feeling unlike themselves. They’re [...]
How to Test Iron Levels in Blood: A Complete UK Guide
You’re probably not searching how to test iron levels in blood out of curiosity. More [...]
Growth Scan Pregnancy: UK Guide & What to Expect
You’re at an antenatal appointment, everything seems routine, and then your midwife says, “We’d like [...]
Gender Scan Near Me: Your 2026 Guide to Options
You’re probably here because the question has stopped feeling abstract. Maybe you’ve had your booking [...]
Progesterone Test For Pregnancy: Viability & Home Kit
The positive test is there, but relief doesn’t always follow. For many women, early pregnancy [...]
Ovulation Blood Tests: Confirm Your Ovulation
You’ve probably already done some version of this. You’ve checked an app, watched for a [...]
How to Test Testosterone Levels: A UK Guide
You wake up tired, despite a full night in bed. Your training feels flat. Your [...]
UK Vitamin D Test: A Complete At-Home Guide for 2026
You wake up tired, even after a full night’s sleep. By mid-afternoon you’re reaching for [...]
Blood Iron Level Test: A Complete UK Guide for 2026
Some days it isn’t dramatic. You’re just slower than usual. You wake up after a [...]
Cortisol Levels Test: Your Comprehensive UK Guide
You wake up tired, push through the morning on caffeine, feel oddly tense by midday, [...]
Travel Clinic Leeds: Compare 7 Top Options For 2026
You book the flights first. Then the practical questions start. Is a tetanus booster enough [...]
Private Blood Test Leicester: A Complete 2026 Guide
You wake up tired again. Maybe you’ve had weeks of bloating, odd fatigue, headaches, low [...]
Genetic Testing Before Pregnancy: A UK Guide for 2026
You might be at the stage where baby plans still live in half-finished conversations. One [...]
Harmony NIPT Test: A Clear Guide for Expectant Parents
You may be sitting with a booking slip from your midwife, a browser full of [...]
Decode Your Health: Understanding Full Blood Count Results
That moment is familiar. You open your blood test report on your phone, see a [...]
Iron Level Tester: Your Guide to Better Health
You wake up tired, push through the day with coffee, and still feel flat by [...]