Peripheral Artery Disease UK: Peripheral Artery Disease UK:
You might be reading this because walking has started to feel different. Perhaps your calf tightens after a few minutes on the high street, then eases when you stop. Or maybe your feet always feel cold and you've put it down to age, weather, or “just poor circulation”.
That's exactly where many people in the UK start with peripheral artery disease uk questions. The tricky part is that PAD can look ordinary at first, yet it can point to a much bigger problem in the arteries.
Understanding Peripheral Artery Disease in the UK
Peripheral artery disease, usually shortened to PAD, happens when arteries that carry blood to the legs and feet become narrowed. Less blood gets through, especially when your muscles need more oxygen during walking or climbing stairs.
In simple terms, your legs are asking for fuel, but the supply line is restricted.
Many people think of PAD as a leg problem only. It isn't that simple. UK reporting from the London School of Economics highlights that PAD carries a high risk of death and disability, including amputation, and that people who develop PAD face a five- to six-fold higher risk of cardiovascular death compared with people without PAD. The same discussion notes that NICE analysis found around 10% to 15% of people diagnosed with PAD die within five years (UK PAD burden and cardiovascular risk summary).
That's why leg pain on walking shouldn't be brushed aside as a minor nuisance.
What PAD often feels like at first
A common pattern is this:
- Walking triggers pain: You walk a certain distance and develop cramp, tightness, or aching in the calf, thigh, or buttock.
- Rest settles it: You stop for a short while and the pain eases.
- The same distance brings it back: It often returns in a repeatable way.
That pattern matters because it's different from random stiffness or a one-off pulled muscle.
PAD isn't just about blood flow to the legs. It can be a warning sign that artery disease is affecting the body more widely.
Why UK patients need a practical explanation
A lot of health content jumps straight to “eat better, stop smoking, exercise more”. That advice matters, but people usually want to know something more immediate first. Could this be PAD, and what happens if I speak to my GP?
That practical UK pathway matters. The NHS often starts with a simple test in primary care or through referral, then decides whether you need further imaging or specialist vascular review. Private care can sometimes shorten that route, but it follows the same basic logic.
What Happens Inside Your Arteries with PAD
Think of an artery like a clean plumbing pipe. When the inside is smooth and open, blood moves through easily. With PAD, the inner lining becomes narrowed by fatty deposits called atheroma. Over time, that narrowing makes it harder for blood to reach the muscles and skin in the lower limbs.
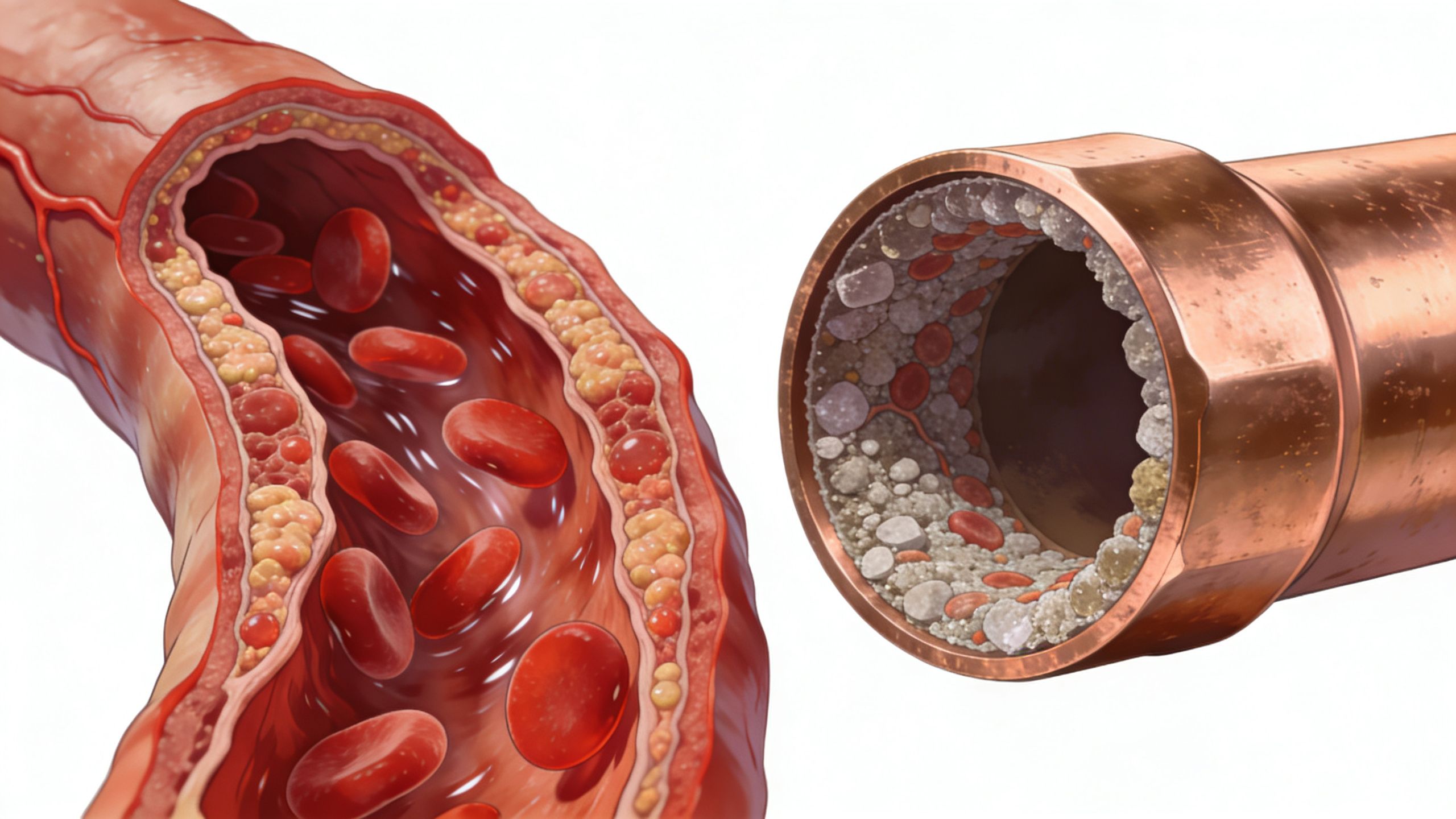
The clogged pipe comparison
If a kitchen pipe narrows, less water gets through. You might not notice much at first when demand is low. Turn on several taps at once, and the problem becomes obvious.
Your legs work in a similar way. At rest, blood flow might be enough. When you walk, especially uphill or at pace, your muscles demand more. If the arteries are narrowed, the gap between supply and demand shows up as pain, heaviness, or cramp.
Why it's not only a leg issue
PAD usually develops through atherosclerosis. That means the same disease process can affect arteries in other parts of the body too. So when someone has PAD, clinicians don't just think about the leg symptoms. They also think about overall vascular health.
That's one reason cholesterol, blood pressure, diabetes control, and smoking status matter so much in this condition. If you're trying to understand your wider cardiovascular picture, this guide to cholesterol levels by age chart can help put one important risk factor into context.
How common PAD is in the UK
PAD is not rare. UK sources estimate that it affects about 1 in 5 people over 60, and that 15% to 20% of adults aged 55 to 75 have objective evidence of lower-extremity PAD (UK PAD prevalence review).
That prevalence changes how you should think about symptoms. If you're older, especially with vascular risk factors, leg pain on walking is common enough to deserve proper assessment rather than guesswork.
The important shift is this. PAD is better understood as a circulation problem in the legs that also signals wider artery disease.
Recognising the Warning Signs and Key Symptoms
The classic PAD symptom is intermittent claudication. That sounds technical, but the pattern is simple. A muscle group in the leg starts to ache, tighten, or cramp during activity, then settles when you stop and rest.
It often affects the calf, though some people feel it higher up in the thigh or buttock.
How PAD pain differs from everyday aches
Ordinary age-related stiffness is usually less predictable. Arthritis can hurt when you first move, then loosen. A muscle strain often stays sore even when you stop. Nerve pain may burn, tingle, or shoot.
PAD pain is often more mechanical than that. The clue is effort brings it on, rest relieves it.
Look for a pattern: if the same walk repeatedly triggers the same leg discomfort, it's worth discussing with a GP.
Symptoms people often miss
PAD doesn't always announce itself clearly. Signs can include:
Common warning signs
- Cramping on walking in the calf, thigh, or buttock
- Cold feet or lower legs compared with the rest of the body
- Slow-healing sores on the feet or lower legs
- Changes in skin colour or texture
- Reduced hair growth or poor nail growth on the legs or feet
- Pain in the foot at rest, especially in more severe disease
Some people dismiss these signs because they seem small on their own. A cold foot here, a stubborn blister there, slightly slower walking pace. Together, they can form a more useful picture.
The symptom problem nobody expects
One of the biggest challenges is that many people with PAD don't notice any obvious symptoms. The Heart Research Institute UK says around 50% of people with peripheral artery disease have no symptoms (PAD symptoms and silent disease overview).
That matters because waiting for dramatic pain isn't a reliable strategy.
If you smoke, have diabetes, high blood pressure, raised cholesterol, or a strong cardiovascular family history, it makes sense to be more alert. You don't need to diagnose yourself. You do need to notice patterns and bring them to a clinician's attention.
Managing Your PAD Risk Factors with At-Home Testing
PAD is closely tied to the same risk factors that damage arteries elsewhere in the body. The main ones people can act on are smoking, high blood pressure, high cholesterol, and diabetes.
The practical question isn't just “Do I have PAD?” It's also “What's increasing my risk, and how do I keep an eye on it?”
The risk factors that do the most damage
- Smoking: Smoking directly harms blood vessels and makes artery disease harder to control.
- High blood pressure: Constant pressure against artery walls contributes to damage over time.
- High cholesterol: Excess cholesterol can contribute to plaque build-up in arteries.
- Diabetes and raised blood sugar: High glucose levels can damage blood vessels and nerves, which can blur the symptom picture and complicate diagnosis.
These factors often overlap. Someone may have no major leg symptoms but still have several vascular risks working together.
Why home monitoring can help
GP care is still central. But in real life, people often wait too long to check basic markers because appointments take time, symptoms feel vague, or life gets in the way.
Home testing can be useful when you want a clearer starting point before or alongside a medical appointment. In the UK, that usually means keeping track of:
- Blood pressure
- Cholesterol and lipid markers
- Longer-term blood sugar markers such as HbA1c
For people worried about diabetes as part of their vascular risk, looking at UK options for diabetes tests can make that process more convenient.
A practical way to use your results
Home results are most useful when you treat them as decision-support, not self-diagnosis.
A sensible approach looks like this:
- Notice a pattern: leg pain on walking, cold feet, slow healing, or known vascular risk factors.
- Check the basics: blood pressure, cholesterol profile, and blood sugar status.
- Take the information to your GP: especially if symptoms persist or your readings are concerning.
- Track changes over time: one reading is a snapshot. Trends are more helpful.
Practical rule: if you've got leg symptoms plus known risk factors, don't wait for symptoms to become severe before asking for assessment.
What home testing can and can't do
Home testing can help you spot risk. It can't confirm PAD on its own.
You still need a clinician to examine pulses, assess symptoms properly, and decide whether you need an ABPI or other vascular tests. But if your blood pressure, cholesterol, or glucose control needs attention, those are worthwhile areas to act on regardless.
How PAD is Diagnosed in the UK NHS and Privately
Diagnosis typically starts with a GP appointment. The GP will usually ask about the pattern of your symptoms, your walking limit, whether the pain settles with rest, and your wider cardiovascular risks. They may also check pulses in your feet and legs and look for skin or nail changes.
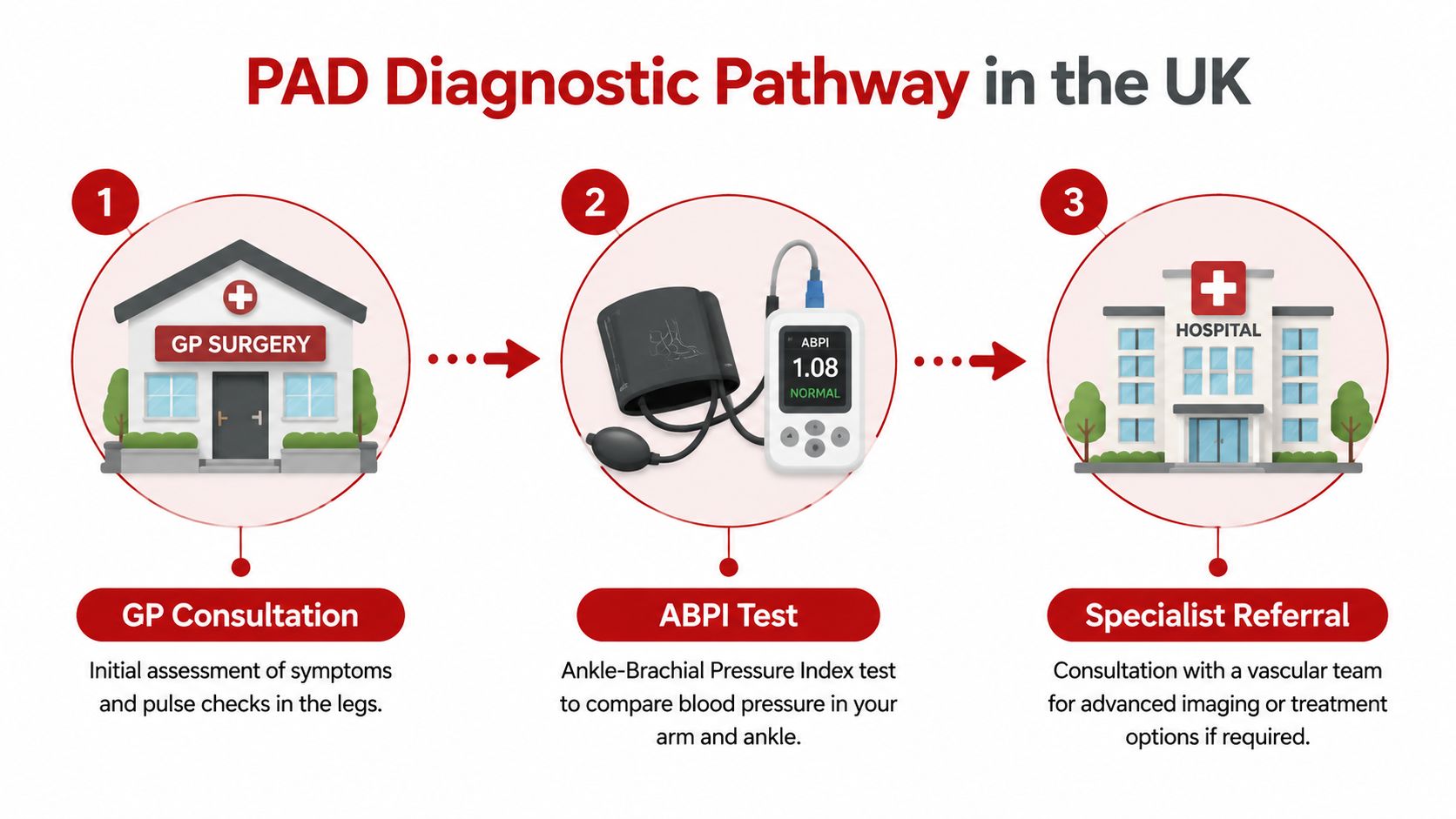
The ABPI test most UK patients hear about
The main first-line test in UK practice is the ankle brachial pressure index, often written ABPI or ABI. It compares blood pressure in your ankle with blood pressure in your arm.
The idea is straightforward. If blood pressure in the ankle is lower than expected compared with the arm, that can suggest narrowing in the arteries supplying the legs.
ABPI is popular because it's non-invasive, relatively quick, and usually enough to help confirm PAD in many routine cases.
Where ABPI can mislead
ABPI is useful, but it isn't perfect. UK cardiology guidance notes that it remains the first-line benchmark, yet interpretation needs care in people with diabetes or calcified arteries. NICE guidance supports ABPI, but experts caution that a normal ABI in the 0.9 to 1.4 range can be misleading in some patients. When symptoms persist despite a normal result, or when diabetes or severe artery calcification is present, further tests such as toe-brachial index or post-exercise ABIs may be needed (UK PAD diagnosis and ABI limitations).
That point confuses a lot of patients. They assume “normal test” means “definitely no PAD”. Sometimes it does. Sometimes it doesn't.
If your symptoms strongly suggest PAD but your first test looks normal, ask what happens next rather than assuming the matter is closed.
What happens after the first assessment
A typical pathway may look like this:
- GP review: symptoms, pulse checks, risk factors, and initial decision-making.
- ABPI testing: often arranged as part of community, practice, or specialist assessment depending on local services.
- Further vascular referral: if symptoms are significant, the diagnosis is uncertain, or intervention is being considered.
When specialists get involved, they may use duplex ultrasound to look at blood flow and identify where narrowing sits. If revascularisation is being considered, more detailed imaging may be discussed.
NHS and private care differences
The NHS route is clinically appropriate for many people, but the pace can vary by area. Some patients move through quickly. Others face waits between GP review, vascular testing, and specialist follow-up.
Private assessment may offer faster access to consultation, ABPI, duplex ultrasound, or vascular review. It doesn't change the biology of PAD, but it can change how quickly you get answers. If symptoms are worsening, you're struggling to walk, or you've had a normal first test that doesn't fit your symptoms, that speed can matter.
Treating PAD Lifestyle Changes and Medical Options
Treatment usually has two aims. First, improve symptoms in the legs. Second, reduce the wider cardiovascular risk that comes with PAD.
Exercise is treatment, not an optional extra
For people whose claudication limits daily life, UK guidance recommends a 12-week supervised exercise programme as first-line treatment, and a review in the UK context found these programmes improve walking distance and quality of life. The same guidance recognises that access is not uniform across the UK, so some patients are left with self-directed walking advice instead (BMJ Best Practice PAD treatment overview).
That uneven access is one of the most frustrating parts of the UK picture. Two patients with similar symptoms may not have the same local options.
If a formal supervised programme isn't available, clinicians often advise a structured home walking plan. Gentle mobility work can also support comfort and movement. If you want simple ideas alongside your main care plan, these exercises on improving circulation for Deerfield Beach patients offer a basic stretching reference that some people find helpful.
What lifestyle treatment usually involves
A strong treatment plan often includes:
- Stopping smoking: this is one of the most important steps if you smoke.
- Regular walking: paced, repeated walking can help improve function over time.
- Heart-healthy eating: useful for cholesterol, blood pressure, and blood sugar control.
- Foot care: especially important if healing is slow or sensation is reduced.
Better vascular health usually comes from repeated small actions, not one dramatic change.
Medicines and procedures
Many patients are also prescribed medicines aimed at the underlying artery disease rather than just the leg pain. Depending on your situation, that may include treatment to lower cholesterol, manage blood pressure, reduce clotting risk, or improve diabetes control.
If symptoms remain severe despite exercise and medication, or if blood supply is badly compromised, specialists may discuss procedures such as angioplasty or bypass surgery. Those options are generally reserved for selected cases, particularly when symptoms are significantly affecting life or when limb health is at risk.
When to push for review
Seek prompt medical advice if pain is worsening, walking distance is shrinking fast, sores aren't healing, or the foot becomes unusually cold, pale, or painful. Those changes suggest you shouldn't just “see how it goes”.
Taking Control of Your Vascular Health Today
PAD is serious, but it's also something you can respond to early.
If walking brings on repeatable calf or leg pain, don't write it off as ageing. If you've got diabetes, high blood pressure, raised cholesterol, or a smoking history, take that risk picture seriously even if your symptoms are mild. And if a first answer doesn't fit what you're feeling, ask whether further testing is needed.
Three practical next steps make a real difference:
- Book a GP appointment if your symptoms match the patterns described above.
- Start a sensible walking routine if you're able, and ask whether supervised exercise is available locally.
- Monitor key risk factors such as blood pressure, cholesterol, and blood sugar.
If you're unsure where to start with one of those basics, this guide on where you can get blood pressure checked is a useful first step.
The aim isn't to become anxious about every ache. It's to notice the patterns that matter and act before they become harder to treat.
Frequently Asked Questions About PAD
A few questions come up again and again when people start looking into peripheral artery disease uk concerns.
Quick answers to common concerns
| Question | Answer |
|---|---|
| Can PAD be reversed? | The artery narrowing itself usually isn't described in simple terms as fully reversible, but symptoms and overall risk can often be improved. Walking programmes, stopping smoking, controlling cholesterol, blood pressure, and diabetes, and using the right medicines can all help. |
| Is PAD the same as varicose veins or poor circulation? | No. Varicose veins involve veins, while PAD involves arteries. People often use “poor circulation” as a catch-all phrase, but PAD has a specific arterial cause and needs proper assessment. |
| Can I have PAD if my legs don't hurt? | Yes. Some people have no obvious symptoms, which is why risk factors and clinical assessment matter. If you have concerns, especially with diabetes or smoking history, ask your GP whether your symptoms and risk profile need further review. |
A useful rule of thumb
If discomfort appears reliably with walking and eases with rest, think artery assessment. If the problem is more about visible bulging veins, swelling, or end-of-day heaviness, the cause may be different. Either way, repeated symptoms deserve a proper evaluation rather than self-diagnosis.
The most helpful question to ask isn't “What do I think this is?” It's “What pattern am I noticing, and who should assess it?”
If you want a convenient way to monitor vascular risk factors from home, Repose Healthcare offers UK at-home health testing with clear instructions, accredited laboratory processing, and secure online results. It's a practical option if you want to check markers such as cholesterol or blood sugar, track your health between appointments, or go into a GP consultation with better information.

You Might Also Like
Peripheral Artery Disease UK: Peripheral Artery Disease UK:
You might be reading this because walking has started to feel different. Perhaps your calf [...]
NIPT Test Cardiff: Clinic, Home & NHS Pathways 2026
If you're in Cardiff, newly pregnant, and staring at screening options that all seem to [...]
Gender Scan Difference UK: Accuracy, Timing & Cost Compared
You've probably already done the same search most parents do. One tab shows the NHS [...]
NIPT Test Cambridge: Guide to Options & Booking 2026
You're in Cambridge, you've had the first rush of finding out you're pregnant, and then [...]
Home COVID Test Results: A Practical UK & Ireland Guide
You've done the swab, mixed the sample, added the drops, and now you're staring at [...]
DVT Test Squeeze Calf: Homan’s Sign & Beyond
You notice one calf is sore, a little swollen, and not behaving like an ordinary [...]
Your Guide to Every Travel Clinic Leicester Offers in 2026
Flights are booked. The hotel is sorted. Your passport is still in date. Then one [...]
13 Week Gender Scan: Accuracy, NIPT & What to Expect
By the time you reach 13 weeks, pregnancy often starts to feel more real in [...]
Your Pregnancy Scan London: Guide to Options & Costs
A positive test can make London feel suddenly very small and very complicated. You might [...]
Your Nuchal Dating Scan Explained: A 2026 UK Guide
That appointment message has landed in your phone or come through the post, and suddenly [...]
Normal Cortisol Levels UK: Get Clarity
Some people search for normal cortisol levels uk after weeks of feeling unlike themselves. They’re [...]
How to Test Iron Levels in Blood: A Complete UK Guide
You’re probably not searching how to test iron levels in blood out of curiosity. More [...]
Growth Scan Pregnancy: UK Guide & What to Expect
You’re at an antenatal appointment, everything seems routine, and then your midwife says, “We’d like [...]
Gender Scan Near Me: Your 2026 Guide to Options
You’re probably here because the question has stopped feeling abstract. Maybe you’ve had your booking [...]
Progesterone Test For Pregnancy: Viability & Home Kit
The positive test is there, but relief doesn’t always follow. For many women, early pregnancy [...]
Ovulation Blood Tests: Confirm Your Ovulation
You’ve probably already done some version of this. You’ve checked an app, watched for a [...]
How to Test Testosterone Levels: A UK Guide
You wake up tired, despite a full night in bed. Your training feels flat. Your [...]
UK Vitamin D Test: A Complete At-Home Guide for 2026
You wake up tired, even after a full night’s sleep. By mid-afternoon you’re reaching for [...]
Blood Iron Level Test: A Complete UK Guide for 2026
Some days it isn’t dramatic. You’re just slower than usual. You wake up after a [...]
Cortisol Levels Test: Your Comprehensive UK Guide
You wake up tired, push through the morning on caffeine, feel oddly tense by midday, [...]
Travel Clinic Leeds: Compare 7 Top Options For 2026
You book the flights first. Then the practical questions start. Is a tetanus booster enough [...]
Private Blood Test Leicester: A Complete 2026 Guide
You wake up tired again. Maybe you’ve had weeks of bloating, odd fatigue, headaches, low [...]
Genetic Testing Before Pregnancy: A UK Guide for 2026
You might be at the stage where baby plans still live in half-finished conversations. One [...]
Harmony NIPT Test: A Clear Guide for Expectant Parents
You may be sitting with a booking slip from your midwife, a browser full of [...]
Decode Your Health: Understanding Full Blood Count Results
That moment is familiar. You open your blood test report on your phone, see a [...]
Iron Level Tester: Your Guide to Better Health
You wake up tired, push through the day with coffee, and still feel flat by [...]
Vitamin D Tests: A UK Guide to Your Results
Some readers land on this topic after a winter of feeling flat out tired. Others [...]
Your DVT Ultrasound Scan: What to Expect in the UK
You may be reading this because one leg suddenly looks different. It may feel tighter [...]
Harmony Test London: NIPT Explained for 2026
If you’re searching for harmony test london, you’re probably in a very specific moment. You [...]
Early Viability Scans: A Complete UK Guide for 2026
That positive pregnancy test can change the feel of an ordinary day in seconds. One [...]