How to Read Blood Test Results UK a Practical Guide in 2026
Getting your blood test results back can feel like you’ve been handed a document in a foreign language, packed with confusing acronyms and numbers. But learning how to read your own blood test results in the UK really just comes down to understanding three things: the name of the marker being tested, your personal result, and the lab’s reference range—what’s considered ‘normal’ for that marker.
This knowledge is powerful. It helps you spot potential issues early and allows you to have much more informed, productive conversations with your GP. An actionable insight from your results could be as simple as changing your diet after seeing high cholesterol, or starting a Vitamin D supplement if your levels are low.
Your Guide to Understanding UK Blood Test Results

Whether you’ve had a test done through the NHS or used a private service, the layout of a lab report can be daunting. It’s a dense document, for sure, but breaking it down makes it far less intimidating. The goal isn’t to diagnose yourself, but to become a proactive partner in your own healthcare by turning data into action.
More and more people are looking to understand their health data. In March 2026, the NHS performed nearly 2.5 million diagnostic tests, a huge 25% jump from pre-pandemic levels. With these volumes, being able to make sense of your own results is an incredibly valuable skill.
Key Terms on Your Report
Every report, whether it’s from your local GP surgery or a provider like Repose Healthcare, will use some specific terminology. Let’s decode the most common terms you’ll encounter.
- Reference Range: This is the range of values that are considered ‘normal’ for a healthy person. It’s important to know these can vary slightly between labs and are often influenced by your age and sex.
- Flag: A result that falls outside the reference range is usually ‘flagged’. You might see a letter next to it (like ‘H’ for high or ‘L’ for low) or an asterisk (*). It’s a simple visual cue to draw your attention to that specific result.
- Units: This tells you how a marker is measured (for example, g/L for haemoglobin or umol/L for creatinine). The units are crucial for comparing results accurately, especially if you get tested by different providers over time.
Practical Example: On a full blood count (FBC), a typical haemoglobin level for a man is between 130-180 g/L. If your result came back as 125 g/L, it would be flagged as low. The actionable insight here is to consider your iron intake or book a follow-up test to investigate potential anaemia.
The real insight comes from tracking your health data over time. A single flagged result might not be clinically significant, but a consistent trend gives a much clearer picture of what’s happening in your body, enabling you to have proactive conversations with your clinician.
This proactive approach is a big reason why the UK’s at-home testing market is growing so quickly, projected to expand from £5036.51 million in 2024 to £9119.51 million by 2033.
Services like ours give you a convenient way to bypass long waiting times and take control of your health monitoring. With our range of online lab tests in the UK, you can get clear, easy-to-understand results delivered straight to a secure dashboard, putting you in the driver’s seat of your own wellness journey.
Diving into Your Full Blood Count (FBC)

The Full Blood Count, or FBC, is one of the most fundamental blood tests we use in the UK. It’s a bit like a general MOT for your blood, giving a broad overview of your health by counting the different cells whizzing around your body. It’s often the first port of call when investigating vague symptoms like feeling wiped out, picking up every bug going, or unusual bruising.
Learning to read your results starts with knowing what an FBC actually looks for. At its core, it examines three main players in your blood: red blood cells, white blood cells, and platelets.
Getting to Know Your Blood Cells
Each of these cells has a very specific job to do. Let’s break down what they are and why they matter.
- Red Blood Cells (RBCs): These are your body’s oxygen couriers. Their star player is a protein called haemoglobin (Hb), which grabs oxygen from your lungs and delivers it to every corner of your body. If your count is low, you’ll likely feel breathless and fatigued.
- White Blood Cells (WBCs): Think of these as the army of your immune system. They’re constantly on patrol, ready to seek and destroy invaders like bacteria and viruses. A high count often means your body is in the middle of a fight.
- Platelets (PLT): These are the tiny first responders. When you get a cut, platelets swarm the area, clumping together to form a plug and stop the bleeding.
Your report will show a value for each of these, measured against a reference range. For example, a typical UK reference range for white blood cells is 4.0–11.0 x10^9/L. A result of 13.5 x10^9/L would be flagged as high, pointing towards a possible infection. An actionable insight would be to rest, hydrate, and re-test in a few weeks if you still feel unwell.
A Real-World Example: Spotting Anaemia
It’s completely natural to feel a jolt of anxiety when you see a result flagged as high or low. But remember, small dips and rises are incredibly common and often mean very little on their own.
Let’s look at a practical scenario. Imagine Sarah has been feeling completely drained for weeks. She decides to order a Repose Healthcare General Health Check, and her FBC comes back with two key markers flagged as low:
- Haemoglobin (Hb): 110 g/L (Reference range for women: 120-160 g/L)
- Red Blood Cell Count (RBC): 3.9 x10^12/L (Reference range: 4.2-5.4 x10^12/L)
This combination—low levels of both her oxygen-carrying protein and the cells that hold it—is a classic pattern for anaemia, often caused by low iron. Instead of causing worry, this result gives Sarah a clear, actionable starting point. She can now have a much more focused conversation with her GP, armed with specific data, and start incorporating more iron-rich foods into her diet.
It’s so important to remember that context is everything. A slightly low white cell count might just be your personal ‘normal,’ while a slightly raised one could be your body getting over a cold. Always look at the bigger picture.
Don’t Sweat the Small Fluctuations
Lots of things can temporarily push your results outside the standard range. These are rarely a sign of anything serious and can include:
- Hydration levels: Being a bit dehydrated can falsely increase your red blood cell count.
- A recent bug: Fighting off a cold will naturally raise your white blood cell count.
- Intense exercise: A hard workout just before your test can throw off a few markers.
- Medications: Many common medicines can have a mild impact on your blood counts.
When looking at your FBC, understanding what each part means—including things like the Platelet Count Test—is vital for getting a complete picture. Minor blips often correct themselves, which is why re-testing to see the trend over time can be so reassuring.
If you are worried about anaemia or just want to establish a healthy baseline, our Iron Status Test or General Health Check provides a simple, convenient way to track these key markers from home.
Interpreting Markers for Your Liver, Kidneys, and Heart
While a Full Blood Count gives you a great snapshot of your overall health, some blood tests dig deeper into how specific organs are doing. Your liver, kidneys, and heart are the body’s real workhorses, ticking away behind the scenes. Monitoring them is a huge part of staying on top of your long-term health.
Let’s break down what the key markers on a UK blood test report actually mean, using real-world examples to help you turn those numbers into meaningful insights.
Your Liver Function Test (LFT)
Think of your liver as a powerhouse factory, handling everything from filtering out toxins to producing bile for digestion. A Liver Function Test (LFT) checks a group of enzymes and proteins in your blood to see how well it’s managing its massive workload.
One of the most common markers you’ll spot is Alanine Aminotransferase (ALT). This is an enzyme that lives mostly inside your liver cells. If those cells get damaged or inflamed, they leak ALT into your bloodstream, and your levels go up.
Practical Example: A typical UK reference range for ALT is under 40 U/L. So, what if your result comes back at 55 U/L? This is a mild elevation. It’s not usually a reason to panic, and could simply be linked to:
- Recent alcohol intake: Even a few nights of heavier drinking can give your ALT a temporary bump.
- Certain medications: Everyday drugs, including paracetamol, can sometimes impact liver enzymes.
- Non-alcoholic fatty liver disease (NAFLD): This condition is becoming increasingly common and is often related to diet and weight.
A single, slightly high reading is more of a nudge to look at your lifestyle than a definite diagnosis. This gives you a clear, data-driven reason to perhaps cut back on alcohol for a few weeks, clean up your diet, and then re-test. You can keep an eye on this marker easily with a dedicated Liver Function Test from Repose Healthcare, letting you track any changes right from home.
Checking Your Kidney Health (U&Es)
Next up: your kidneys, the body’s sophisticated filtration plant. A Urea and Electrolytes (U&Es) test is the go-to for checking how well they’re working by measuring waste products and essential minerals in your blood.
The marker to watch here is Creatinine. It’s a waste product created by muscle activity, and a healthy pair of kidneys should filter it out of your blood efficiently. If your kidneys start struggling, creatinine levels begin to creep up.
A rising creatinine level is a key indicator of declining kidney function. It’s a silent marker, meaning you often won’t have symptoms until significant damage has already occurred, which makes regular monitoring so valuable.
Practical Example: Imagine your report shows a creatinine of 115 umol/L (a typical male range is 62-106 umol/L), flagging it as high. While things like having a lot of muscle mass or being a bit dehydrated can nudge it up, a result that stays high is an actionable insight prompting you to discuss it with your GP. It’s a solid piece of evidence that can help guide any further checks.
Understanding Your Lipid Profile for Heart Health
Your lipid profile is all about the fats circulating in your blood, and these are directly tied to your risk of developing heart disease or having a stroke. This panel looks at a few different types of cholesterol.
Here’s a quick guide to what you’re looking at:
- Total Cholesterol: This is the overall amount of cholesterol in your blood. Ideally, you want this to be below 5.0 mmol/L.
- LDL Cholesterol (The ‘Bad’ One): This is the type that can clog up your arteries by forming plaques. The target here is a level below 3.0 mmol/L.
- HDL Cholesterol (The ‘Good’ One): This helpful type of cholesterol works to clear the bad stuff away. You want this number to be higher, ideally above 1.0 mmol/L for men and 1.2 mmol/L for women.
Practical Example: Let’s say your results show a high LDL of 4.2 mmol/L and a low HDL of 0.9 mmol/L. This combination is a pretty clear warning sign for your cardiovascular risk. Your actionable insight is to make tangible changes like increasing fibre intake, reducing saturated fats, and boosting your physical activity.
Worryingly, many people are walking around with less-than-ideal cholesterol levels and have no idea. Research has shown a majority of people have at least one biomarker outside the optimal range, even if they feel fine. This is especially true for heart health, with data showing that over 70% of those aged 60+ have suboptimal cholesterol. With NHS data identifying an extra 289,383 patients at high cardiovascular risk in 2025-2026, knowing your numbers has never been more important. You can read more about these population health trends in this detailed report from Medichecks.
At-home kits like our Advanced Heart Health Test give you a direct way to track these crucial markers, especially when getting a routine diagnostic appointment through the NHS can involve long waits.
Analysing Hormones, Nutrients and Inflammation
Beyond organ function, your blood test results can tell you a lot about your body’s messaging systems (hormones) and the essential building blocks it runs on (nutrients). When you’re feeling ‘off’, tired, or just not yourself, these are often the first things to go out of balance.
Interpreting these markers gives you a fascinating window into your overall wellbeing. It’s no surprise that people are taking a more active role in their health. The UK blood testing market is predicted to grow significantly, from USD 5.04 billion in 2024 to USD 9.12 billion by 2033, and at-home testing is a huge part of that shift.
Decoding Your Thyroid Function
Think of your thyroid gland, the small butterfly-shaped organ in your neck, as your body’s metabolic engine. A Thyroid Function Test (TFT) is one of the most common blood tests for checking how well this engine is running. It usually measures a few key hormones.
- Thyroid-Stimulating Hormone (TSH): Produced in your brain, TSH tells your thyroid to get to work. A high TSH level can suggest your thyroid isn’t responding as it should, a classic sign of an underactive thyroid (hypothyroidism).
- Free T4 (FT4): This is the main hormone your thyroid produces. It’s ‘free’ because it’s available for your body to use.
- Free T3 (FT3): This is the more active thyroid hormone, converted from T4. It’s the one that directly controls your metabolism.
Practical Example: Imagine your TSH comes back at 5.2 mIU/L. A typical reference range is 0.5–4.5 mIU/L, so this result would be flagged as high. It suggests your brain is having to "shout" at your thyroid to produce more hormones. This is a common indicator of hypothyroidism, which could explain symptoms like fatigue and weight gain. The actionable insight is to schedule a GP appointment to discuss this result.
A TSH result is often the first clue that something is amiss with your thyroid. Even a result at the upper end of the ‘normal’ range can be significant if you have symptoms, making it a vital marker to track.
Our Advanced Thyroid Test measures TSH, FT4, and FT3, giving you a complete picture of your thyroid’s performance. It’s an easy way to investigate nagging symptoms or monitor a known condition from the comfort of your home.
Key Nutrients and Vitamins
Certain nutrients are notoriously low across the UK population, and even minor deficiencies can have a huge impact on your energy and mood. Blood tests are the only real way to know for sure what your levels are.
Vitamin D: Often called the ‘sunshine vitamin’, it’s vital for bone health and immune function. With our limited sun exposure in the UK, deficiency is widespread.
- Practical Example: A level of 24 nmol/L points to a clear deficiency. Your actionable insight is to start a daily vitamin D supplement and aim to get your level above 75 nmol/L on your next test.
Vitamin B12: This is essential for nerve function and making red blood cells. A B12 deficiency can cause profound fatigue and ‘brain fog’.
- Practical Example: A result under 150 ng/L is typically considered deficient. This result would prompt you to speak to your GP about B12 supplementation and review your diet.
Checking these levels is simple. Our targeted Vitamin B12 Test or a broader wellness panel can quickly reveal if a deficiency is the culprit behind your symptoms. It’s also worth looking into other nutrients; for example, depending on your results, you might explore the benefits of taking zinc before bed to support overall health and sleep.
Inflammation and Other Key Markers
Finally, some markers provide a wider view of what’s happening inside your body, especially when it to comes to inflammation.
C-Reactive Protein (CRP): This is a general marker for inflammation. A high level, usually over 10 mg/L, shows there’s inflammation somewhere, but it doesn’t tell you the cause.
Ferritin: This protein is responsible for storing iron in your body. Low ferritin is often the very first sign of iron deficiency.
- Practical Example: If you’re a woman with a ferritin level of 20 µg/L, this is an actionable insight to increase iron-rich foods and consider an iron supplement, especially if you experience fatigue. You can learn more by reading our guide on the ferritin blood test in the UK. For women with heavy periods, our Endometriosis Blood Test can also provide valuable insights.
UK Reference Ranges for Common Health Markers
The table below provides a guide to the typical reference ranges for some of the key markers we’ve discussed. It’s important to remember that these ranges can vary slightly from one lab to another, and your own ‘normal’ might be different. Always look at the reference range provided on your specific report.
| Biomarker | Typical UK Reference Range | What It Indicates |
|---|---|---|
| TSH | 0.5 – 4.5 mIU/L | Thyroid function |
| Free T4 (FT4) | 10 – 22 pmol/L | Thyroid hormone production |
| Vitamin D | 50 – 200 nmol/L (Optimal >75) | Bone and immune health |
| Vitamin B12 | 200 – 900 ng/L | Nerve function, energy |
| Ferritin | 30 – 300 µg/L (Men), 15 – 150 µg/L (Women) | Iron storage levels |
| CRP | < 5 mg/L | General inflammation |
These ranges are a great starting point for understanding your results, but they are just one piece of the puzzle. The most important thing is to view them in the context of your symptoms and overall health.
Turning Your Results Into an Action Plan
Getting your blood test results back is the first step. The real value, though, comes from knowing what to do with that information. A single test is just a snapshot in time, but tracking your markers over several months or years tells the real story of your health. This is how you move from just reading numbers to building a solid, personal health plan.
This is exactly what the Repose Healthcare dashboard was designed for. Instead of seeing one isolated number for your cholesterol, you can actually see how it’s trending. Has it been slowly creeping up? Or have those changes you made to your diet started to bring it down? This trend data is far more powerful than a one-off result.
Spotting Red Flags vs. Amber Flags
Once you have your report, the next job is to sort through the results. A key part of learning how to read your own blood test results is knowing the difference between a ‘red flag’ and an ‘amber flag’.
- Red Flags: These are results that are seriously outside the normal range and could signal an urgent problem. They need prompt medical attention. A classic example is a very high potassium level (hyperkalaemia), which can disrupt your heart’s rhythm and means an immediate call to your GP or even a trip to A&E.
- Amber Flags: Think of these as early warnings. They’re mild or moderate changes that aren’t an emergency but are telling you something needs attention. Slightly raised cholesterol or a borderline high HbA1c are perfect examples of amber flags. They’re a clear signal to look at your diet and lifestyle and plan a re-test.
This flowchart gives a great visual of the decision-making process for TSH, a key thyroid marker.
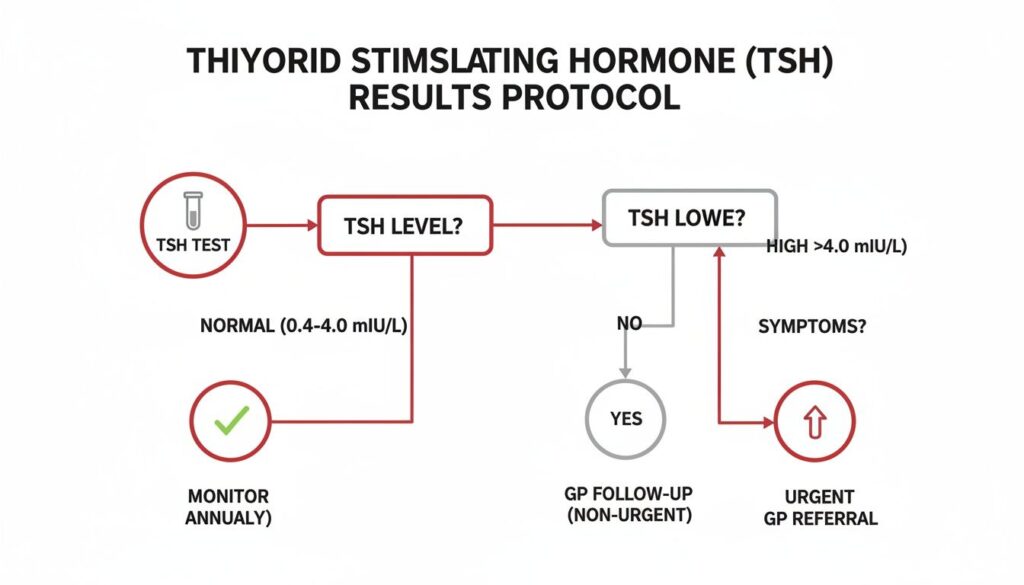
As you can see, a normal TSH means you can continue to monitor, but a high result is a definite reason to book in with your GP to find out what’s going on.
How to Have a Productive Chat with Your GP
If your results do need a discussion with a doctor, going in prepared can make a world of difference. It’s much more effective than just saying "my blood test was a bit off." You can lead the conversation with specifics.
Walking into your GP’s office with a clear timeline of your results and a list of specific questions transforms the dynamic. You become an active participant in your healthcare, working with your doctor to find the best path forward.
Here’s a quick checklist to help you get ready:
- Bring your results: Have your Repose dashboard open on your phone or bring a printout. It helps to highlight the specific markers you’re concerned about.
- Connect the dots with your symptoms: Link the numbers to how you’ve been feeling. For instance, "My ferritin has been dropping over the last six months, and I’ve been feeling more and more tired and breathless."
- Mention any recent changes: Have you started a new medication, changed your diet, or been under a lot of stress? This context is absolutely vital for your doctor.
- Write down your questions: It’s easy to forget things in the moment. Good questions to ask are, "Given this result, what do you think the next steps should be?" or "Should we plan to re-test this in a few months?"
Practical Example: If you took our Advanced Heart Health Test and saw your LDL cholesterol was high, you could show your GP the trend data, ask for advice on lifestyle changes, and discuss if a follow-up test in three months is a sensible plan.
The entire Repose Healthcare service is built to support you through this. From your dashboard, you can easily order a follow-up test to keep an eye on an ‘amber flag’ or dive into our blog for more information. It puts all the tools you need to manage your health in one secure, easy-to-use place.
Common Questions About UK Blood Test Results
Even after you start to get the hang of reading your blood test results, it’s completely normal to have a few more questions. Nailing down these finer details is what helps you turn those abstract numbers into real, practical knowledge about your health.
Here are the answers to some of the most common queries we hear from people just starting to track their health markers.
Why Do Reference Ranges Differ Between Labs?
You’ve probably noticed that the ‘normal’ reference range on an NHS report might look slightly different to one from a private provider like Repose Healthcare. Don’t worry, this is perfectly normal and happens for a couple of key reasons:
- Different Kit and Methods: Labs use slightly different analytical machines and chemical reagents to process samples, which can cause tiny variations in the final numbers.
- Local Population Data: A lab often sets its reference ranges based on what’s considered ‘normal’ for the healthy local population in their specific area.
The most important takeaway is to always use the reference range printed on your specific report. A result flagged as ‘high’ on one report will still be high on another, even if the exact numbers vary a little.
A good way to think about it is like regional accents. The words might sound slightly different depending on where you are, but the underlying meaning is the same. Just interpret your results in the context of the lab that produced them.
Why Do I Need to Fast for Some Blood Tests?
Fasting before a blood test can feel like a bit of a pain, but for certain markers, it’s absolutely essential for getting an accurate result. The main reason is that food and drink can temporarily alter the levels of specific substances in your blood, giving a misleading picture of your health.
The most common tests that require fasting include:
- Glucose Tests: Used to check your blood sugar levels and screen for diabetes. Eating will naturally raise your glucose, so a fasting sample gives a true baseline reading.
- Lipid Profile (Cholesterol): A fatty meal can send your triglyceride levels soaring for several hours, which would completely skew an assessment of your heart health.
Fasting usually means no food or drink (except for water) for 8-12 hours before your sample is taken. If a test needs you to fast, the instructions will make this crystal clear.
How Often Should I Get Routine Blood Work?
For a generally healthy adult with no specific symptoms or chronic conditions, getting a comprehensive wellness check every one to two years is a sensible approach. This helps you establish your personal baseline and spot any slow-moving trends before they turn into a problem.
Of course, this changes if you’re actively managing a condition (like a thyroid disorder or high cholesterol), have a strong family history of certain illnesses, or are making big lifestyle changes. In those cases, your GP might suggest more frequent testing, perhaps every three to six months.
This is where at-home testing really comes in handy, giving you the flexibility to re-test key markers on your own schedule. For more on this, you can check out our guide on how long blood test results take and how to plan your testing frequency.
At Repose Healthcare, we believe that understanding your health data is the first step towards improving it. Our convenient at-home tests, secure dashboard, and clear, expert-reviewed results are all designed to support you on your wellness journey. Take control of your health today by exploring our full range of tests.


You Might Also Like
Peripheral Artery Disease UK: Peripheral Artery Disease UK:
You might be reading this because walking has started to feel different. Perhaps your calf [...]
NIPT Test Cardiff: Clinic, Home & NHS Pathways 2026
If you're in Cardiff, newly pregnant, and staring at screening options that all seem to [...]
Gender Scan Difference UK: Accuracy, Timing & Cost Compared
You've probably already done the same search most parents do. One tab shows the NHS [...]
NIPT Test Cambridge: Guide to Options & Booking 2026
You're in Cambridge, you've had the first rush of finding out you're pregnant, and then [...]
Home COVID Test Results: A Practical UK & Ireland Guide
You've done the swab, mixed the sample, added the drops, and now you're staring at [...]
DVT Test Squeeze Calf: Homan’s Sign & Beyond
You notice one calf is sore, a little swollen, and not behaving like an ordinary [...]
Your Guide to Every Travel Clinic Leicester Offers in 2026
Flights are booked. The hotel is sorted. Your passport is still in date. Then one [...]
13 Week Gender Scan: Accuracy, NIPT & What to Expect
By the time you reach 13 weeks, pregnancy often starts to feel more real in [...]
Your Pregnancy Scan London: Guide to Options & Costs
A positive test can make London feel suddenly very small and very complicated. You might [...]
Your Nuchal Dating Scan Explained: A 2026 UK Guide
That appointment message has landed in your phone or come through the post, and suddenly [...]
Normal Cortisol Levels UK: Get Clarity
Some people search for normal cortisol levels uk after weeks of feeling unlike themselves. They’re [...]
How to Test Iron Levels in Blood: A Complete UK Guide
You’re probably not searching how to test iron levels in blood out of curiosity. More [...]
Growth Scan Pregnancy: UK Guide & What to Expect
You’re at an antenatal appointment, everything seems routine, and then your midwife says, “We’d like [...]
Gender Scan Near Me: Your 2026 Guide to Options
You’re probably here because the question has stopped feeling abstract. Maybe you’ve had your booking [...]
Progesterone Test For Pregnancy: Viability & Home Kit
The positive test is there, but relief doesn’t always follow. For many women, early pregnancy [...]
Ovulation Blood Tests: Confirm Your Ovulation
You’ve probably already done some version of this. You’ve checked an app, watched for a [...]
How to Test Testosterone Levels: A UK Guide
You wake up tired, despite a full night in bed. Your training feels flat. Your [...]
UK Vitamin D Test: A Complete At-Home Guide for 2026
You wake up tired, even after a full night’s sleep. By mid-afternoon you’re reaching for [...]
Blood Iron Level Test: A Complete UK Guide for 2026
Some days it isn’t dramatic. You’re just slower than usual. You wake up after a [...]
Cortisol Levels Test: Your Comprehensive UK Guide
You wake up tired, push through the morning on caffeine, feel oddly tense by midday, [...]
Travel Clinic Leeds: Compare 7 Top Options For 2026
You book the flights first. Then the practical questions start. Is a tetanus booster enough [...]
Private Blood Test Leicester: A Complete 2026 Guide
You wake up tired again. Maybe you’ve had weeks of bloating, odd fatigue, headaches, low [...]
Genetic Testing Before Pregnancy: A UK Guide for 2026
You might be at the stage where baby plans still live in half-finished conversations. One [...]
Harmony NIPT Test: A Clear Guide for Expectant Parents
You may be sitting with a booking slip from your midwife, a browser full of [...]
Decode Your Health: Understanding Full Blood Count Results
That moment is familiar. You open your blood test report on your phone, see a [...]
Iron Level Tester: Your Guide to Better Health
You wake up tired, push through the day with coffee, and still feel flat by [...]
Vitamin D Tests: A UK Guide to Your Results
Some readers land on this topic after a winter of feeling flat out tired. Others [...]
Your DVT Ultrasound Scan: What to Expect in the UK
You may be reading this because one leg suddenly looks different. It may feel tighter [...]
Harmony Test London: NIPT Explained for 2026
If you’re searching for harmony test london, you’re probably in a very specific moment. You [...]
Early Viability Scans: A Complete UK Guide for 2026
That positive pregnancy test can change the feel of an ordinary day in seconds. One [...]