A lot of people search for a sti testing kit uk after the same kind of evening. You notice a symptom. Or maybe you don’t have symptoms at all, but there’s a new partner, a condom split, or a nagging feeling that it’s time to check. You want answers, but you may not want a waiting room, a phone call, or a conversation at reception.
That’s a sensible reaction. Sexual health testing should feel straightforward, private, and manageable. Home testing has made that possible for many people, especially those who want discretion or who can’t easily get to a clinic during working hours.
Anna is a good example of how this usually starts. She feels well, but she’s recently started seeing someone new. She knows regular testing is part of looking after herself, yet she keeps putting it off because booking an appointment feels awkward and inconvenient.
That delay is common. It doesn’t mean someone is careless. It usually means life is busy, privacy matters, and sexual health still feels more personal than most other routine checks.

Home testing changes the experience. Instead of rearranging your day around a clinic visit, you can collect samples in your own bathroom, post them back, and read your results in private. If you’ve looked at other areas of digital care, the wider shift is similar to other telehealth innovations that bring healthcare closer to home.
The need for easier access is real. In 2024, England recorded 364,750 new STI diagnoses, which shows why accessible testing still matters, especially because untreated infections can lead to longer-term problems such as infertility, according to this UK STI statistics overview.
Some people want privacy. Others want speed. Many want the process to feel less stressful.
A home kit can help if you:
Testing isn’t just for people with symptoms. It’s also for people who want certainty.
If you’re comparing options, some people start with broader online lab tests in the UK so they can choose a kit that matches their concern rather than guessing.
The biggest shift is psychological. You’re not waiting for someone else to tell you when you can test. You’re taking action yourself.
That matters because sexual health isn’t just about reacting to a problem. It’s about keeping routine checks easy enough that you’ll do them.
A good home kit is basically a lab-in-a-box. Every item has one job. Once you know what each piece is for, the whole process feels much less intimidating.
Open the pack and you’ll usually find a small set of collection tools, instructions, return materials, and labels or activation details. The exact contents depend on which infections the panel checks for, because different tests need different sample types.
Most private STI kits include some combination of the following:
Not all STIs are tested in the same way. That’s why one kit may look simple and another may include several sample devices.
A basic screen often focuses on common bacterial infections and may rely on urine or a swab. A broader panel may add finger-prick blood collection to check for infections such as HIV or syphilis that aren’t reliably covered by a urine-only approach.
That’s where people often get confused. They assume one sample should detect everything. It can’t.
Practical rule: Match the kit to the infections you want checked, not just the cheapest option on the page.
The best kits are organised in the order you need them. You shouldn’t have to guess which tube goes with which sample.
Look for:
A simple way to think about it is this. The kit doesn’t ask you to do laboratory work. It asks you to collect a sample correctly, package it safely, and send it back. The lab handles the technical side.
| Item | What it does | Why it matters |
|---|---|---|
| Swab or urine tube | Collects the sample | The right sample type supports reliable testing |
| Lancet and blood tube | Collects a blood sample if needed | Some infections need blood-based testing |
| Instructions | Guides the process | Reduces mistakes and rejected samples |
| Activation details | Links sample to you | Ensures results go to the right account |
| Return packaging | Sends sample to the lab | Protects the sample and keeps the process simple |
Once you’ve seen the contents in this way, the kit stops feeling medical and starts feeling practical.
A common question is whether a home test is reliable? In the UK, many home STI kits use the same core lab methods clinics use, so the answer depends less on “home versus clinic” and more on whether the sample is collected and processed properly.
At-home STI kits use Nucleic Acid Amplification Tests (NAATs), the same technology as clinics, achieving over 95% sensitivity and more than 99% specificity in UKAS-accredited labs, with self-collected samples showing comparable accuracy to clinician-collected ones when instructions are followed, as explained by Vitall’s guide to female STI testing.
That sentence contains a lot of jargon, so let’s make it simple.
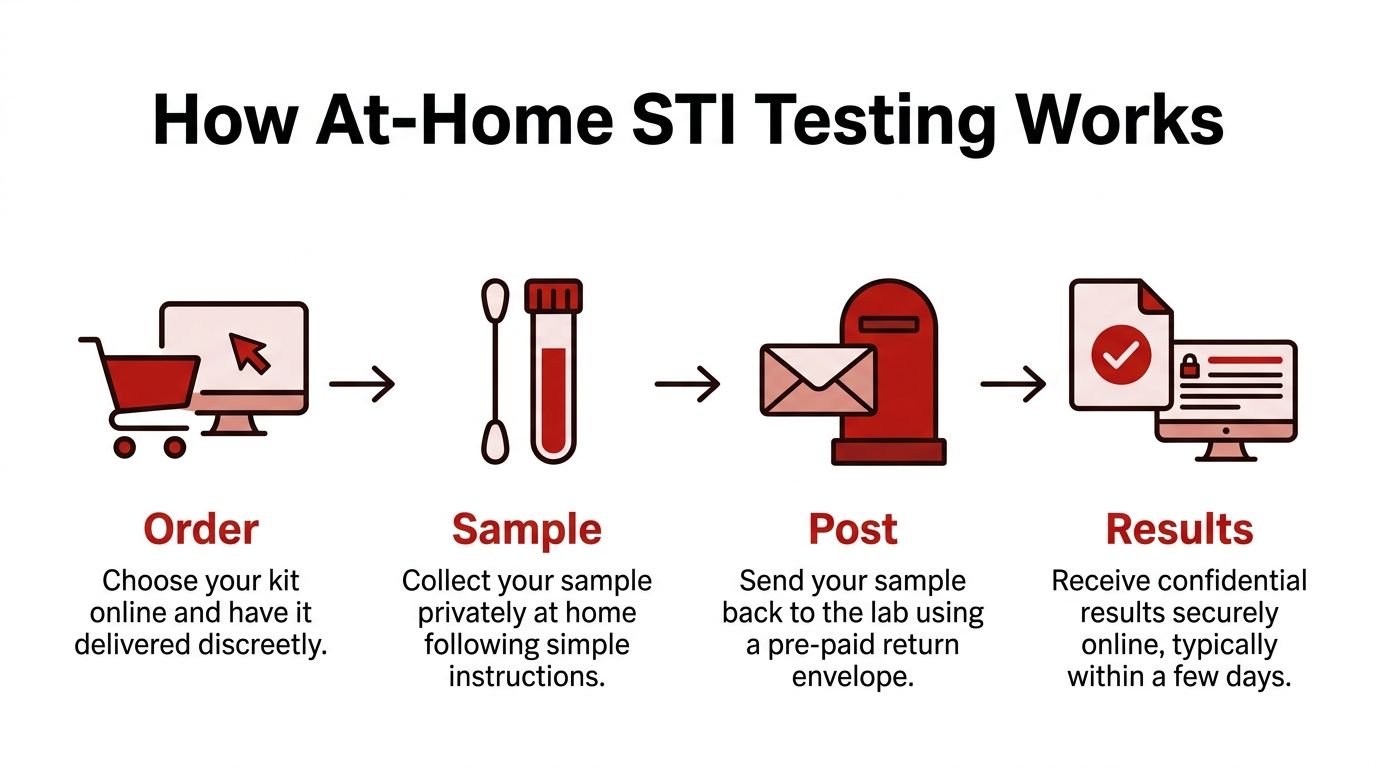
The process usually follows four stages.
Order
You choose a test panel online. The kit arrives in discreet packaging.
Sample
You collect urine, a swab, blood, or a combination, depending on the panel.
Post
You seal the sample using the packaging provided and return it with the prepaid mailer.
Results
The lab analyses the sample and your results are released through a secure online account.
These terms sound technical, but the idea is straightforward.
For someone using a sti testing kit uk, that means a well-designed test is built to detect what it should detect and avoid unnecessary false alarms. The accuracy still depends on correct sampling, which is why the instructions matter so much.
A home kit is only one part of the chain. The lab matters just as much.
A UKAS-accredited laboratory works to recognised quality standards. That includes how samples are received, stored, processed, checked, and reported. For you, that means the result isn’t based on a quick strip test done in your kitchen. It’s based on laboratory analysis performed after you send the sample back.
If the sample collection is the front end, the accredited lab is the engine.
Different infections are more reliably detected from different sample types. In plain terms:
A useful example is this. If someone only orders a urine-based test after oral or anal exposure, that may not give a full picture. The sample has to match the likely exposure site.
The journey from your letterbox to your result depends on a few practical details:
Private services can feel easier here because the process is built around speed. Clear instructions, prepaid tracked returns, and secure online reporting cut out a lot of friction.
Most errors aren’t about the science. They’re about the handling.
Common issues include:
None of these are hard to avoid once you know them. That’s why a carefully read instruction leaflet often makes the difference between a smooth result and a repeated test.
The hardest part usually isn’t taking the test. It’s deciding which one to trust.
Search results are full of options. Some look almost identical. The price points vary, the panels vary, and the language can be vague. If you want a reliable sti testing kit uk, a quick checklist helps you filter out weak options fast.
A basic panel may be suitable if you only need a focused check for common bacterial infections. A more complete panel becomes important when you want broader reassurance or your exposure history is less clear.
Thorough panels matter because early HIV detection through p24 antigen or syphilis can be missed by basic tests, and self-sampling has been shown to boost testing uptake by 40% among high-risk groups, according to LetsGetChecked’s overview of complete STI testing.
That’s the key buying decision. Ask yourself whether you want a narrow answer or a wider one.
Here’s a simple way to think about the options many buyers compare.
| Feature | Basic STI Test | Advanced STI Test | Full STI Screen |
|---|---|---|---|
| Typical focus | Chlamydia and gonorrhoea | Adds broader bacterial coverage | Adds blood-based infections such as HIV and syphilis |
| Sample type | Usually urine or swab | May include multiple swabs or urine | Often combines swab or urine with finger-prick blood |
| Best for | Targeted routine checks | Broader screening after mixed exposure | People who want the widest home-based picture |
| Main limitation | Doesn’t cover everything | May still not include full blood markers | More involved collection process |
| Buyer question | “Do I need a simple check?” | “Do I need more than the basics?” | “Do I want one kit that covers more ground?” |
If you’re comparing specific options, you can order STI test online and review what each panel includes before choosing.
A trustworthy kit should make quality standards easy to find.
Look for these signs:
If those details are hidden, incomplete, or written in vague marketing language, that’s a warning sign.
Free testing through regional services is valuable, but it isn’t always available to everyone who wants it. Some schemes are limited by postcode, age, or the exact type of test offered.
That matters when you need a nationwide option, want a broader panel, or don’t meet local eligibility rules. Private kits fill that gap because you can choose the service based on your needs rather than your location.
Fast results aren’t just about convenience. They affect what you do next.
If you’re anxious, waiting longer can be the hardest part of the process. If a result is positive, quicker reporting also means you can move sooner towards treatment, partner notification, or further medical advice.
Before you buy, ask:
A cheap kit that skips blood testing, hides lab details, or limits access can end up costing more in stress and repeat testing.
Take two buyers. One had vaginal exposure only and wants a straightforward routine screen. A basic kit may be enough. Another had mixed exposure and wants reassurance about HIV and syphilis as well as common bacterial STIs. That person usually needs a more thorough panel, not just a cheaper urine-only option.
The right choice depends on the question you need answered.
This is the part people worry about most. In practice, it’s usually simpler than expected once you slow down and follow the order on the leaflet.
The most important first step is easy to miss. Activate the kit before you collect anything if your provider requires activation. That links the barcode or reference number to your secure account. If you skip that step, the lab may not be able to match the sample to you.
Regional access can also affect who reaches this stage at all. Free NHS self-sampling schemes often have strict age or location rules, with some services limited to residents of a specific area aged 16+, which creates a gap that private nationwide services can fill, as shown on Umbrella Health’s self-sampling information page.
Set yourself up properly first.
For urine testing, timing and technique matter.
A common mistake is overthinking it and using a random clean container from home first. Don’t. Use the collection materials that came with the kit.
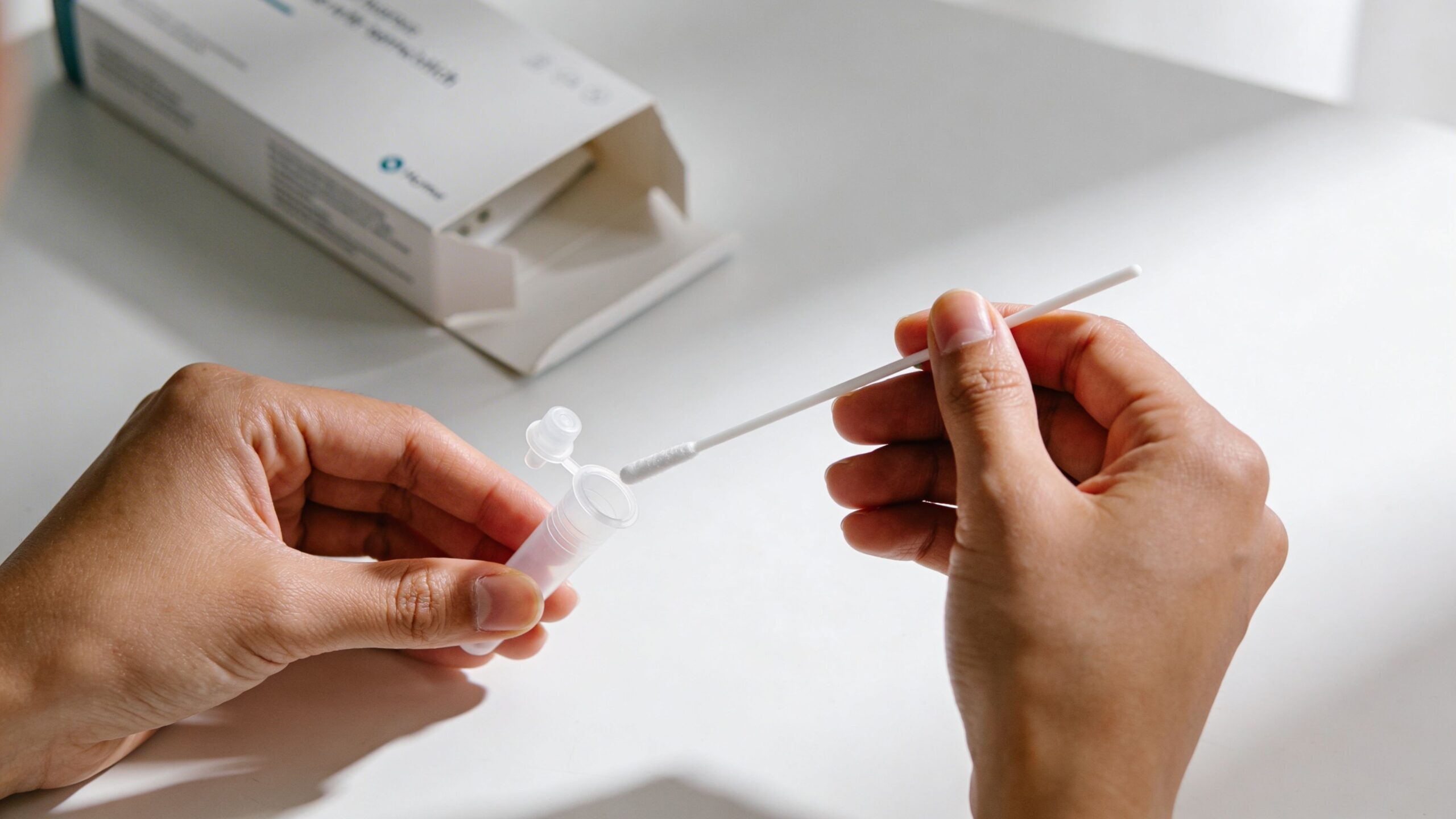
This sounds more daunting than it usually is.
If your hands are cold, collection often takes longer. That’s one of the most common avoidable frustrations.
Cold hands are the enemy of a finger-prick sample. Warm them before you start, not halfway through.
Swabs vary by site, so always follow the kit-specific leaflet. The general principles are similar.
Open the swab without touching the tip. Collect the sample as instructed, place the swab into the tube, and snap or seal it if required.
Avoid touching the swab tip to your tongue, teeth, or other surfaces unless the instructions tell you otherwise. Return it straight to the tube after collection.
Take your time and follow the guide closely. The aim is a correct sample, not speed.
Once the samples are collected:
| Mistake | Why it causes trouble | Better approach |
|---|---|---|
| Forgetting activation | Sample may not link to your account | Activate before collecting |
| Waiting too long to post | Sample quality may be affected | Post as soon as possible |
| Touching the swab tip | Can contaminate the sample | Handle swabs by the stem |
| Too little blood | Lab may not have enough to analyse | Warm hands and allow time |
| Mixing up tubes | Can delay or invalidate testing | Lay out all items first |
If you’re ever unsure during collection, pause and re-read the leaflet. Taking an extra minute is better than repeating the whole test.
The result screen is the moment many have been waiting for. It’s also where calm, clear wording matters most.
You’ll usually see results reported in simple terms such as Detected or Not Detected. That language can feel blunt, so it helps to translate it into everyday meaning.
Not Detected means the lab didn’t find evidence of the infection tested for in that sample. Detected means the lab found evidence consistent with that infection and you should arrange appropriate follow-up care.
A negative result is reassuring, but context still matters.
Think about:
A negative result is most useful when the right test was taken at the right time using the right sample.
Take a breath first. A positive result is something to act on, not something to panic about.
Your next steps are usually straightforward:
A positive STI result is a health task. It is not a judgement about you.
This is one reason many people choose private testing. With rising cases of syphilis and gonorrhoea, wide-ranging testing matters, and while some NHS services have a 7-day average for results, private providers such as Repose Healthcare can return results in 1-3 days, as noted in UKHSA guidance on getting tested for an STI.
That shorter wait can make a practical difference. It gives you less time spent worrying and more time to take the next sensible step.
If you want a clearer sense of timing, this guide on how long STI test results take can help you understand what affects turnaround.
Try not to jump beyond what the report says.
That’s why good sexual health care combines the result, your symptoms, your exposure history, and the timing of the test.
They can be, if the kit uses proper laboratory methods and you collect the sample correctly. The sample is taken at home, but the analysis is done in an accredited lab, not guessed from a home strip result.
If you have symptoms, especially pain, sores, discharge, bleeding, or fever, it’s sensible to seek medical advice rather than relying only on a home kit. A clinician may want to examine you, choose the right sample site, or rule out something that isn’t an STI.
A window period is the time after exposure when an infection may not yet show up reliably on a test. That’s why timing matters. If you test too early, you may need to test again later based on the instructions for that kit or advice from a clinician.
No. Some kits are narrow and some are broad, but no single sample type answers every question. A urine-only kit, for example, won’t replace blood testing when blood-based analysis is needed.
Usually, yes. Good providers use plain packaging and secure online accounts so your order and results stay private. If privacy matters to you, check the packaging and reporting details before buying.
Yes, that’s one reason private kits are useful. Regional free schemes can have postcode or age limits, while private options are generally designed for broader access.
The lab may report that the sample was insufficient or unsuitable. That can happen with too little blood, the wrong collection method, or packaging mistakes. Reading the leaflet first lowers the chance of that.
Choose based on your need. If your concern is limited and specific, a basic panel may be enough. If you want wider reassurance, have had mixed exposure, or are concerned about infections that require blood testing, a more thorough panel often makes more sense.
They should be. Look for a GDPR-compliant results system and clear privacy information from the provider.
If you want a private, straightforward way to check your sexual health from home, Repose Healthcare offers UK and Republic of Ireland at-home lab testing with discreet delivery, prepaid returns, and secure online results.